 |
 |
- Search
| Clin Exp Reprod Med > Volume 50(1); 2023 > Article |
|
Abstract
Objective
The aim of this study was to investigate the relationships of serum folate (vitamin B9), cobalamin (vitamin B12) levels and diet with semen parameters (semen standard parameters [SSP] and DNA fragmentation index [DFI]) in infertile men.
Methods
Sperm samples were assessed for SSP and DFI (using the sperm chromatin dispersion test). Serum vitamin concentrations were measured with an immuno-electrochemiluminescence assay, and men completed a semi-quantitative food frequency questionnaire (FFQ).
Results
Serum folate levels were positively correlated with sperm progressive motility and DFI. A comparison of SSP between two groups of patients according to serum folate concentration (B9 <4.840 ng/mL and B9 Ōēź4.840 ng/mL) showed significantly higher sperm concentration and sperm progressive motility in the latter group. However, there was no difference between these groups regarding DFI. Interestingly, serum folate levels were significantly higher in patients with a high DFI (using the cut-offs of 30% or 18%). FFQ data showed that the consumption of fruits and egg yolk correlated positively with sperm concentration and sperm motility, respectively.
Infertility is an important health concern worldwide. Approximately 15% of couples do not achieve pregnancy within a year of regular unprotected sexual intercourse [1]. It is estimated that up to 50% of infertility cases are due to male reproductive disorders [2]. However, the etiology of failure to conceive remains unknown in 30% of infertile men [3].
Beyond semen standard parameters (SSP), sperm DNA integrity is also associated with fertility. Nevertheless, the routine analysis of sperm DNA fragmentation (SDF) is not yet a common practice [4]. Studies are actively being conducted to understand the role of DNA and chromatin integrity, as well as exogenous factors such as lifestyle, in human fertility. Therefore, diet has been a core focus of many studies in the last decade.
Indeed, many biological processes in male and female fecundity depend on compounds derived from the diet [5]. Furthermore, substantial changes in dietary behavior can induce serious malformations in offspring [6]. At the molecular level, micronutrients such as folate (vitamin B9), riboflavin (vitamin B2), niacin (vitamin B3), cobalamin (vitamin B12), and zinc play fundamental roles as substrates or cofactors in DNA synthesis and methylation within the one-carbon cycle [7,8]. Hence, many studies, reviews, and meta-analyses have investigated the relationship between fertility and diet. However, most of the literature comprises studies that were carried out in Western countries or in Asia, and studies are still scarce in Africa, particularly in North Africa, which is characterized by distinctive dietary patterns.
Among the micronutrients, vitamins B9 and B12 are water-soluble vitamins that are involved in DNA metabolism. Vitamin B9 plays the role of a coenzyme in one-carbon metabolism, which is necessary for deoxythymidylate synthesis, purine synthesis and various methylation reactions [9-11]. Vitamin B12 is involved in general (together with its coenzymatic form, methylcobalamin) in the reactions that lead to de novo synthesis of thymidine, essential for DNA replication and repair [12].
The aim of this study was to investigate the relationship between food consumption, as estimated by a semi-quantitative food frequency questionnaire (FFQ) and the blood concentration of vitamins (folate and cobalamin), as well as the relationship of vitamin concentrations with SSP and SDF. This study was conducted among infertile men from a North African population, providing novel insights on the relationship of the specific diet of this region with male infertility.
A total of 29 infertile men were included in this cross-sectional study. These patients underwent routine semen and blood analyses as part of biological investigations of their infertility at Ibn Rushd Laboratory of Medical Analysis. Obtaining a larger sample was hindered by the fact that patients often consider collecting a semen sample for analysis to be awkward and embarrassing. Information on smoking, alcohol consumption, and chemical exposure during occupational activities was collected through a questionnaire. The study was approved by the Institutional Consultative Committee of Ethics of the National Center for Biotechnology Research (CRBt). All the participants provided informed written consent.
Approximately 64% of the patients suffered from primary infertility. All but two patients had engaged in at least 1 year of regular unprotected sexual intercourse with their partners. For those two patients, semen analysis had revealed a case of asthenozoospermia for one and azoospermia for the other.
Semen was obtained by masturbation after a period of sexual abstinence of 3 to 5 days. Semen samples were collected in sterile containers and liquefied at 37┬░C within 30 minutes.
After liquefaction, semen volume, pH, and viscosity were assessed. According to the World Health Organization guidelines [13], the reference values were as follows: volume Ōēź1.5 mL, pH Ōēź7.2, and normal viscosity.
Concentration, motility, and morphology were measured using a semen quality analyzer (VideoTesTŌĆōSperm 2.2 software, VideoTest Ltd., St. Petersburg, Russia) that was connected to an optical microscope (model MT4300L, Meiji Techno Co., Ltd, Saitama, Japan) coupled to a ProgRess camera microscope (Jenoptik, Jena, Germany). An aliquot of 2 ┬ĄL of the semen sample was deposited on a disposable counting chamber (Leja Products, Nieuw Vennep, Netherlands) measuring 10 ┬Ąm in height. Many fields of the sample were examined to reach a total of 200 spermatozoa. May-Grunwald-Giemsa staining was used to evaluate the morphology.
Oligozoospermia was diagnosed when the sperm concentration was less than 15 million/mL. The lower limit of normal sperm morphology was 4% and if the progressive motility (PM) was less than 32%, the diagnosis of asthenozoospermia was established [13].
The DNA fragmentation was assessed by a sperm chromatin dispersion test using a Halosperm G2 kit (Halotech, Madrid, Spain). Briefly, fragmented sperm DNA is denatured by an acid. Following this, a second treatment that consists of a lysis solution removes nuclear proteins. When there is slight or no DNA breakage, a halo is observed around the sperm head that is absent in sperm with degraded DNA. The halo is very small when there is meaningful DNA damage [14,15].
According to the manufacturerŌĆÖs instructions, the semen sample was diluted to obtain a maximum of 20 million sperm per milliliter. Then, 100 ╬╝L of agarose was melted at 95┬░C to 100┬░C for 5 minutes and then transferred to a temperature of 37┬░C for 5 minutes. After that, 50 ╬╝L of semen was mixed with agarose, and 8 ╬╝L of the cell suspension (semen and agarose) was deposited on the treated side of the slide on a cold surface and covered with 24├Ś24 mm coverslip. Next, the slide was transferred into a refrigerator at 4┬░C for 5 minutes. The coverslip was removed and the cell suspension was incubated in the denaturation solution (solution 1) for 7 minutes. After removing the reagent, the slide was incubated in the lysis solution (solution 2) for 20 minutes. When solution 2 had been removed, the slide was washed with abundant distilled water for 5 minutes. Incubation in 70% ethanol followed by 100% ethanol was applied for 2 minutes each . After drying, Diff-Quik staining was used to allow visualization under a bright field microscope (model MT4300L). SDF was estimated after counting at least 300 sperm cells to calculate the DNA fragmentation index (DFI), as suggested in previous research [15]:
The average of DFI from two slidesŌĆÖ readings was calculated unless there was a notable difference between the two readings. In this case, a third reading was necessary.
Before collecting the blood samples, patients were asked to fast for at least 8 hours. The blood was collected in a dry tube and centrifuged at 2,000├Śg to obtain serum samples. Folate and cobalamin concentrations in blood serum were calculated using an automated immuno-electrochemiluminescence assay, which is a competitive assay (Cobas E601, Roche Diagnostics, Basel, Switzerland), following the manufacturerŌĆÖs instructions. Briefly, a first step in dissociating the serum vitamin from its carrier protein is performed and followed by the addition of ruthenium, which binds to the carrier protein. Subsequently, biotinylated vitamin and streptavidin microparticles were added to the mixture. The subsequent chemiluminescence reaction allowed the quantification of the ruthenium-carrier protein complex, which is proportional to the quantity of the tested vitamin.
Participants completed a FFQ containing the food categories that were studied in a National Health Survey [16]. It was developed in order to estimate the frequency and the consumption of foods known to be rich in folate and cobalamin during the precedent year. The FFQ was filled out by the patients themselves. This FFQ consisted of 76 food items, including traditional meals, distributed into 10 categories: cereals and pasta; meat, seafood; vegetables, fruits, legumes; dairy products and eggs; sweets (including biscuits, donuts, and pastries [traditional, pies, cakes, etc.]), nuts (referring to any hard-walled, edible kernel); and seasonal foods.
The frequency of consumption was expressed by scores from 0 to 12 as follows: 0, never; 1, once a year; 2, 2ŌĆō5 times per year; 3, 6ŌĆō11 times/year; 4, once a month; 5, 2ŌĆō3 times/month; 6, once a week; 7, twice a week; 8, 3ŌĆō4 times/week; 9, 5ŌĆō6 times/week; 10, once daily; 11, twice daily; and 12, three or more times/day. For seasonal foods, the scores were from 0 to 11 as follows: 0, never; 1, once a season; 2, twice a season; 3, once a month per season; 4, 2ŌĆō3 times/month in the season; 5 once a week in the season; 6, twice a week in the season; 7, 3ŌĆō4 times/week in the season; 8, 5ŌĆō6 times/week in the season; 9, once daily in the season; 10, twice daily in the season; and 11, three or more times/day in the season. The questionnaire was provided on the day of semen and blood collection and was returned on the day when the participant received the results.
To assess the relationships between different parameters of semen, blood, and nutrients, Spearman correlation coefficients were calculated. The non-parametric Mann-Whitney U test was used for comparisons between groups with high and low values of semen or blood parameters. We conducted the analysis by setting the cut-off value of DFI to 18% and then to 30%, as recommended in previous studies [17,18], respectively. Data were expressed as median (range) with a 95% confidence interval (CI). The threshold for statistical significance was set as p<0.05. Analyses were performed using GraphPad Prism version 7.00 (GraphPad Software, San Diego, CA, USA).
The general characteristics of the study population, the sperm parameters, and serum vitamin levels are summarized in Table 1. The median and range of age and body mass index were, respectively, 35 years (range, 24ŌĆō50) and 26.0 kg/m2 (range, 18.9ŌĆō36.9). The median abstinence time was 3 days (range, 3ŌĆō5).
The median value of PM (18.25%) was lower than the reference limit (32%). Half of the studied population has asthenozoospermia, 25% were oligoasthenozoospermic, and 7.14% were azoospermic. Teratozoospermia was found in 3.57% of participants.
We found that 86.21% of men had a serum folate concentration less than the inferior limit of the normal range adopted in the laboratory (4.840ŌĆō14.960 ng/mL), while only 20.69% of the patients had a serum vitamin B12 concentration less than the reference value (191ŌĆō946 pg/mL). A significant correlation was also observed between serum folate and PM (r=0.396; 95% CI, ŌĆō0.002 to 0.685; p=0.045) (Table 2). However, there was no correlation between SSP and the serum concentration of vitamin B12.
We compared the SSP values between patients with serum folate (vitamin B9) levels <4.840 or Ōēź4.840 ng/mL, according to the threshold of the normal value according to the clinical laboratory instructions. We found a significant difference between these groups in the sperm concentration (22├Ś106/mL [range, 0ŌĆō121] vs. 50├Ś106/mL [range, 35ŌĆō89], p=0.0308) and PM (17.4% [range, 0%ŌĆō40.3%] vs. 32.7% [range, 30.1%ŌĆō51.9%], p=0.0169). The same comparison of two other groups of patients distributed according to the serum vitamin B12 status (B12 <191.0 pg/mL and B12 Ōēź191.0 pg/mL) did not show a significant difference. The results of the different comparisons are summarized in Table 3.
There was no significant difference in DFI between the two groups of patients distributed according to the folate or the vitamin B12 threshold (Table 3). However, a strong correlation was found between serum folate and DFI (r=0.517; 95% CI, 0.151ŌĆō0.759; p=0.0068) (Table 2). When patients were grouped according to a DFI threshold of Ōēż18% versus >18%, a significant difference was found in folate concentrations (1.35 ng/mL [0.42ŌĆō10.49] vs. 2.75 ng/mL [0.66ŌĆō10.90], p=0.0459) (Figure 1). The same comparison was carried out, but with a DFI threshold of 30% (DFI Ōēż30% and DFI >30%) (Figure 1). Once again, the only observed difference was in folate concentrations, but with a higher degree of significance (1.765 ng/mL [0.42ŌĆō10.49] vs. 3.375 ng/mL [1.85ŌĆō10.90], p=0.0084), confirming the results of the serum folate and DFI correlation analysis (Table 2).
Table 4 shows the results of the correlation analysis for each group of food items with either serum vitamin (folate and vitamin B12), the SSP, and the DFI. A positive correlation was found between the serum vitamin B12 concentration and the consumption of organ meat (also called ŌĆ£offalŌĆØ) (r=0.464; 95% CI, 0.039ŌĆō0.747; p=0.0297) and between the consumption of fruit and the sperm concentration (r=0.503; 95% CI, 0.091ŌĆō0.769; p=0.0169). There was also a negative correlation between folate concentration and sweets consumption (r=ŌĆō0.458; 95% CI, ŌĆō0.743 to ŌĆō0.032; p=0.032).
Table 5 shows the results of the same correlation analysis, but taking into consideration food items that were quite rich in folate (liver, breakfast cereal, egg yolk, lettuce, spinach, and nuts [any hard-walled, edible kernel]) or in vitamin B12 (liver, fish, shrimp, Camembert cheese, or egg yolk). We found an association between PM and egg yolk consumption (r=0.478; 95% CI, 0.031ŌĆō0.766; p=0.033) and between vitamin B12 and the consumption of Camembert cheese (r=0.423; p=0.0498) (Table 5).
In this study, we assessed the relationships between the serum concentrations of two vitamins implicated in DNA metabolism (folate and vitamin B12) and food consumption, as well as with SSP and SDF, in the context of male infertility. To the best of our knowledge, this is the first study to study the associations of all these parameters at the same time. In addition, our study included a diet from the North African region. The North African diet is based on traditional dishes and is characterized by its diversity and a high intake of fruits, vegetables, fish, and unsaturated fat.
Most of the men in our study suffered from at least one SSP anomaly, and most of them had deficient folate status. We have found that SSP (specifically, sperm concentration, and PM) are associated with serum folate concentrations. This is in line with previous studies that found positive correlations between sperm concentration and serum folate levels and demonstrated that folate deficiency impaired spermatogenesis [19]. A recent systematic review and meta-analysis concluded that an association exists between paternal folate status and sperm quality [20]. It is interesting that sperm folate levels are 1.5 times higher than serum folate levels [21], and both concentrations are correlated [22]. Hence, we can speculate that our results can be explained by the higher concentration of sperm folate and its effects on spermatogenesis.
However, we did not find any significant associations between SSP and serum vitamin B12 concentrations. The same result was reported by Boxmeer et al. [23] and Murphy et al. [24], but Boxmeer et al. [23] described a correlation between SSP and semen cobalamin instead. This correlation between SSP and the seminal (and not the serum) levels of cobalamin has been recently reported in the context of morbid obesity [25]. Nonetheless, the effect of cobalamin supplementation on sperm parameters remains unclear. Even though a review [26] concluded that vitamin B12 can improve sperm count and motility, the absence of any vitamin B12 influence has been reported in many other studies. In a recent preliminary study [27], combination therapy of antioxidant supplements, including vitamin B12, only improved sperm motility. In our study population, we compared biochemical and seminal parameters between the patients who took vitamin supplementation (including vitamins B9 and B12) and those who did not. The differences were not significant (data not shown). Therefore, it seems that other factors might influence the association of serum vitamin B12 levels with SSP. Cobalamin metabolism is complex and includes several turning points, any of which may be polymorphic between individuals. For instance, the correlation of cobalamin concentrations between blood and semen suggests its transfer between the two compartments. Hence, studying molecular variability in this transfer will be very interesting.
We found a surprising positive correlation between serum folate and DFI. Few studies are available on the relationship between circulating folic acid and SDF in humans. The only available study [23] showed no correlation between them, but reported a negative correlation between seminal folate and DFI. Most of the literature is about the effect of folate supplementation on SDF. In the same vein as our study, a recent study showed an increase of SDF following high-dose folic acid supplementation (5 mg daily intake, corresponding to more than 10 times the 400 ╬╝g recommended daily allowance) for 6 months, combined with zinc [28]. The same high-dose did not show a significant effect on SDF, but altered the human sperm methylome in another study. This alteration was influenced by the common MTHFR C677T polymorphism [29], which emphasizes the importance of the personal genetic background. It also seems that the dose and duration of folate supplementation affect the way it may influence SDF. Indeed, a recent study confirmed the usefulness of folate supplementation (0.8 mg daily for 3 months) in improving sperm quality, including DNA integrity [30], while a quite similar dose (1 mg daily) but for a longer period (6 months) with other antioxidants failed to show such an effect in another study [31]. Furthermore, a smaller folate dose (0.2 mg daily treatment), even for a duration of 6 months, failed to decrease DFI [32]. In the most recent systematic review that investigated the effect of antioxidant supplementation (together with folate) on semen quality (including SDF) [33], only two studies considered folate and SDF at the same time. Both studies showed that the consumption of a mixture of antioxidants including folate (0.2 mg daily for 3 months) improved sperm DNA integrity [34,35]. In addition to differences in doses and duration of vitamin treatment, and in an attempt to explain all these discrepancies, we can also speculate that these differences may be due to the heterogeneity of the studies and the different sizes of study populations, the use of folate alone or combined with other antioxidants (e.g., zinc or lipoic acid); or polymorphisms in participantsŌĆÖ genes that are involved in folate metabolism. Larger prospective studies comparing multiple arms (with different doses and durations of supplementation) and taking into account participantsŌĆÖ genetic backgrounds would provide insights into the real relationship between folate intake and SDF.
Our semi-quantitative FFQ revealed some interesting correlations that are in accordance with the trends of many studies. For instance, serum folate levels correlated positively with the consumption of egg yolk. Even though vegetables lead the way as a source of folate, eggs are a valuable source as well [36]. We did not find a correlation between serum folate and vegetable or fruit consumption, but we found a positive correlation between the consumption of fruits (known to be rich in vitamins and antioxidants) and sperm concentration. Interestingly, we found that folate levels correlated negatively with sweets consumption. We can speculate that the latter may hinder the efficiency of folate absorption from food because additives such as citrate (widely largely used in sweets) can inhibit the intestinal brush border pteroylpolyglutamate hydrolase, which is required to deconjugate polyglutamyl folate to monoglutamyl folate, a mandatory step prior to absorption [37]. Additionally, we noticed a positive correlation between organ meat or Camembert cheese consumption with serum cobalamin levels. Indeed, cobalamin is produced solely by bacteria and archaea, and the presence of such microorganisms is predominant in animal products [38]. Globally, our FFQ results are in accordance with the trends of many studies. When evaluating the effects of folate and B12 dietary intake, as estimated by a semi-quantitative FFQ, on semen parameters, Najafipour et al. [39] found that higher intake of these vitamins than the cut-offs for the recommended daily intake (B9 Ōēź0.4 mg, B12 Ōēź2.4 ╬╝g) significantly improved sperm concentration and motility in men with the T allele of the MTHFR gene. However, recent reviews reported inconclusive results regarding the effect of dietary patterns on male infertility. For example, a healthy dietary pattern (like seafood, poultry, whole grains, legumes, skim milk, fruits, and vegetables) could be or not be related to improvements in SSP or SDF [40-42]. Nonetheless, most studies have converged toward a negative impact of unhealthy Western dietary patterns that are rich in fats, red and processed meats, refined grains, sweets and sweetened beverages, pizza, snacks, and mayonnaise. A large study that enrolled 7,282 men from an Asian population [43] showed that the intake of a highly Westernized diet, high consumption of sweet snacks and sugar-sweetened drinks, a high-carbohydrate diet, and a high-sodium diet were associated with decreased sperm concentration, normal sperm morphology, total motility, and PM. Other authors found that the risk of asthenozoospermia could be minimized by a healthy diet [44].
Adding more complexity, it is noteworthy that people do not consume isolated nutrients because diets may contain chemical factors that may improve or impair the fertility potential. Despite the fact that foods like meat, dairy, seafood, fruits, and vegetables are quite rich in vitamins, the effect of toxic residues that they may contain should not be ignored. It has been argued that total fruit and vegetable intake is directly not associated with SSP, but rather that poor-quality SSP may be associated with a high intake of pesticide residue in fruits and vegetables [45]. Interestingly, an evaluation of the pesticide residues in fruits and vegetables showed that, for some pesticides, the acute reference dose was exceeded [46]. Similarly, the presence of estrogens in cow milk was confirmed, and their association with poorer semen quality was established in some studies [47]. In addition, processed meat (by adding chemical preservatives) intake was associated with a lower total sperm count and total PM count [48]. The methylmercury contamination of fish and shellfish is well known [49], as well as the high risk of infertility in men with elevated blood and hair mercury concentrations [50,51]. Hence, the effects of chemical factors may also contribute to some discrepant results between the studies of dietary factorsŌĆÖ associations with sperm quality.
In addition to the influence of the quantity of nutrients and the quality of food, the dysregulation of nutrient transport in the body may influence their biological effects. For example, despite an adequate intake of B12-containing food sources, the hypothesis of malabsorption of this vitamin cannot be discarded [52]. As well, passive or active transport of folate and vitamin B12 from blood to the testis has been proposed [23].
In our study, we found a significant correlation between serum folate concentrations and SSP. The positive correlation between DFI and blood folate concentrations is another interesting finding, which is in line with other recent studies. Hence, we recommend a careful prescription of vitamin supplements (especially folate) in infertile men. A healthier diet should be advised instead. Alternatively, a randomized controlled trial on the effect of folate supplementation on DFI could be recommended in our population. The limitations of our study are a lack of information on semen vitamin concentrations and on patientsŌĆÖ genetic status regarding the main actor proteins in folate and cobalamin metabolism. Therefore, it would be warranted to conduct larger studies that would more exhaustively explore factors such as diet, genetic background, and folate and cobalamin levels in both serum and semen.
Acknowledgments
We thank the entire Ibn Rochd Laboratory staff for their technical assistance, as well as Drs. Habib Madjor and Abdelhamid Benchadi for their help.
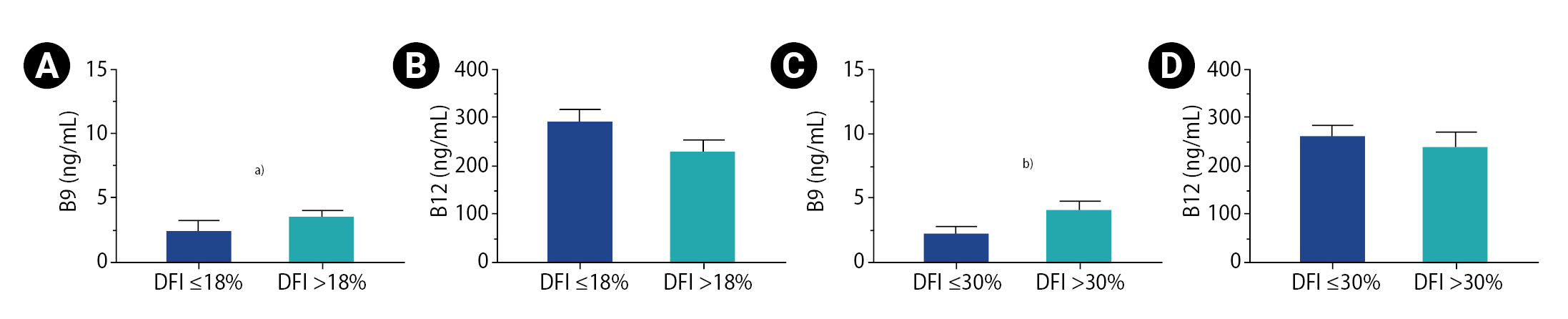
Figure┬Ā1.
Comparison of vitamin concentrations according to DNA fragmentation index (DFI). (A) Concentration of vitamin B9 in the 18% threshold groups. (B) Concentration of vitamin B12 in 18% threshold groups. (C) Concentration of vitamin B9 in the 30% threshold groups. (D) Concentration of vitamin B12 in the 30% threshold groups. Superior limits of boxes represent means; whiskers represent the standard error of the mean. a)p<0.05; b)p<0.01.
Table┬Ā1.
General characteristics of men, sperm parameters, and serum vitamin concentrations
Table┬Ā2.
Association between semen parameters and vitamins
| Concentration | Progressive motility | Normal morphology | DFI | |
|---|---|---|---|---|
| B9 | 0.361 (ŌĆō0.025 to 0.654) | 0.396a) (ŌĆō0.002 to 0.685) | ŌĆō0.062 (ŌĆō0.449 to 0.344) | 0.517b) (0.151 to 0.759) |
| B12 | 0.036 (ŌĆō0.4132 to 0.352) | ŌĆō0.143 (ŌĆō0.511 to 0.270) | 0.042 (ŌĆō0.361 to 0.433) | ŌĆō0.170 (ŌĆō0.532 to 0.244) |
Table┬Ā3.
Comparison of SSP and DFI according to the concentration of vitamins
| Parameter |
B9 |
B12 |
||||
|---|---|---|---|---|---|---|
| <4.840 ng/mL | Ōēź4.840 ng/mL | p-value | <191.0 pg/mL | Ōēź191.0 pg/mL | p-value | |
| Sperm concentration (├Ś106/mL) | 22 (0ŌĆō121) | 50 (35ŌĆō89) | 0.031a) | 25.5 (7.0ŌĆō43.0) | 24 (0ŌĆō121) | 0.945 |
| Sperm progressive motility (%) | 17.4 (0ŌĆō40.3) | 32.7 (30.1ŌĆō51.9) | 0.017a) | 15.8 (4.3ŌĆō51.9) | 20.2 (0ŌĆō40.3) | 0.708 |
| Normal sperm morphology (%) | 50.0 (0ŌĆō65.4) | 52.4 (47.1ŌĆō 62.5) | 0.431 | 48.3 (0ŌĆō62.5) | 51.2 (38.1ŌĆō65.4) | 0.778 |
| DFI (%) | 22.9 (2.8ŌĆō90) | 37.95 (5.3ŌĆō44.5) | 0.704 | 30.7 (5.3ŌĆō71.4) | 18.74 (2.8ŌĆō90) | 0.355 |
Table┬Ā4.
Correlation of food group consumption with blood and sperm parameters
| Food group | Vitamin B9 | Vitamin B12 | Concentration | PM | Normal morphology | DFI |
|---|---|---|---|---|---|---|
| Cereals and pasta | 0.271 (ŌĆō0.184 to 0.629) | 0.05 (ŌĆō0.391 to 0.472) | 0.252 (ŌĆō0.202 to 0.617) | 0.242 (ŌĆō0.238 to 0.627) | 0.194 (ŌĆō0.285 to 0.595) | 0.155 (ŌĆō0.321 to 0.569) |
| Legumes | ŌĆō0.079 (ŌĆō0.494 to 0.366) | 0.087 (ŌĆō0.359 to 0.500) | 0.168 (ŌĆō0.285 to 0.560) | ŌĆō0.130 (ŌĆō0.551 to 0.344) | 0.184 (ŌĆō0.295 to 0.588) | 0.256 (ŌĆō0.224 to 0.636) |
| Vegetables | 0.24 (ŌĆō0.215 to 0.609) | ŌĆō0.141 (ŌĆō0.540 to 0.311) | 0.361 (ŌĆō0.085 to 0.686) | 0.282 (ŌĆō0.197 to 0.652) | ŌĆō0.280 (ŌĆō0.651 to 0.199) | ŌĆō0.035 (ŌĆō0.481 to 0.425) |
| Fruits | 0.254 (ŌĆō0.201 to 0.618) | 0.125 (ŌĆō0.325 to 0.529) | 0.503a) (0.091 to 0.769) | 0.366 (ŌĆō0.105 to 0.703) | 0.209 (ŌĆō0.270 to 0.606) | 0.217 (ŌĆō0.262 to 0.611) |
| Meat | ŌĆō0.317 (ŌĆō0.659 to 0.134) | 0.353 (ŌĆō0.094 to 0.682) | ŌĆō0.305 (ŌĆō0.652 to 0.147) | 0.044 (ŌĆō0.418 to 0.488) | ŌĆō0.169 (ŌĆō0.579 to 0.308) | ŌĆō0.194 (ŌĆō0.596 to 0.285) |
| Organ meat | ŌĆō0.051 (ŌĆō0.473 to 0.390) | 0.464a) (0.039 to 0.747) | 0.131 (ŌĆō0.320 to 0.533) | 0.196 (ŌĆō0.283 to 0.597) | ŌĆō0.304 (ŌĆō0.666 to 0.174) | ŌĆō0.269 (ŌĆō0.644 to 0.210) |
| Seafood | ŌĆō0.053 (ŌĆō0.475 to 0.388) | 0.206 (ŌĆō0.248 to 0.586) | 0.125 (ŌĆō0.325 to 0.529) | 0.208 (ŌĆō0.272 to 0.604) | ŌĆō0.061 (ŌĆō0.501 to 0.404) | 0.126 (ŌĆō0.348 to 0.548) |
| Dairy | ŌĆō0.395 (ŌĆō0.707 to 0.045) | 0.127 (ŌĆō0.324 to 0.530) | 0.029 (ŌĆō0.408 to 0.456) | ŌĆō0.006 (ŌĆō0.458 to 0.449) | 0.243 (ŌĆō0.237 to 0.628) | 0.03 (ŌĆō0.429 to 0.478) |
| Eggs | ŌĆō0.176 (ŌĆō0.565 to 0.278) | ŌĆō0.204 (ŌĆō0.585 to 0.251) | 0.084 (ŌĆō0.361 to 0.499) | 0.198 (ŌĆō0.281 to 0.598) | 0.056 (ŌĆō0.408 to 0.497) | 0.268 (ŌĆō0.211 to 0.644) |
| Sweets | ŌĆō0.458a) (ŌĆō0.743 to ŌĆō0.032) | 0.119 (ŌĆō0.330 to 0.525) | ŌĆō0.220 (ŌĆō0.596 to 0.235) | ŌĆō0.180 (ŌĆō0.586 to 0.298) | 0.014 (ŌĆō0.443 to 0.465) | ŌĆō0.160 (ŌĆō0.572 to 0.317) |
| Nuts | 0.084 (ŌĆō0.362 to 0.498) | ŌĆō0.003 (ŌĆō0.435 to 0.430) | 0.202 (ŌĆō0.253 to 0.583) | 0.354 (ŌĆō0.119 to 0.696) | 0.379 (ŌĆō0.090 to 0.711) | 0.236 (ŌĆō0.244 to 0.623) |
Table┬Ā5.
Correlation of some food items that are quite rich in folate or cobalamin with blood and sperm parameters
| Food item | Vitamin B9 | Vitamin B12 | Concentration | PM | Normal morphology | DFI |
|---|---|---|---|---|---|---|
| Breakfast cereal | 0.019 (ŌĆō0.417 to 0.448) | NA | ŌĆō0.070 (ŌĆō0.487 to 0.374) | 0.316 (ŌĆō0.161 to 0.673) | 0.01 (ŌĆō0.446 to 0.462) | 0.045 (ŌĆō0.417 to 0.489) |
| Lettuce | 0.039 (ŌĆō0.400 to 0.464) | NA | 0.253 (ŌĆō0.201 to 0.618) | ŌĆō0.057 (ŌĆō0.498 to 0.407) | ŌĆō0.093 (ŌĆō0.525 to 0.377) | 0.215 (ŌĆō0.265 to 0.609) |
| Spinach | ŌĆō0.033 (ŌĆō0.459 to 0.405) | NA | ŌĆō0.141 (ŌĆō0.541to 0.310) | 0.141 (ŌĆō0.334 to 0.559) | ŌĆō0.081 (ŌĆō0.516 to 0.387) | 0.258 (ŌĆō0.222 to 0.637) |
| Liver | ŌĆō0.067 (ŌĆō0.485 to 0.376) | 0.418 (ŌĆō0.017 to 0.721) | 0.155 (ŌĆō0.298 to 0.550) | 0.18 (ŌĆō0.298 to 0.586) | ŌĆō0.224 (ŌĆō0.616 to 0.255) | ŌĆō0.293 (ŌĆō0.659 to 0.185) |
| Organ meat | ŌĆō0.051 (ŌĆō0.473 to 0.390) | 0.464a) (0.039 to 0.747) | 0.131 (ŌĆō0.320 to 0.533) | 0.196 (ŌĆō0.283 to 0.597) | ŌĆō0.304 (ŌĆō0.666 to 0.174) | ŌĆō0.269 (ŌĆō0.644 to 0.210) |
| Fish | NA | 0.142 (ŌĆō0.310 to 0.541) | 0.138 (ŌĆō0.313 to 0.538) | 0.227 (ŌĆō0.253 to 0.617) | ŌĆō0.020 (ŌĆō0.469 to 0.438) | 0.165 (ŌĆō0.312 to 0.576) |
| Shrimp | NA | ŌĆō0.327 (ŌĆō0.665 to 0.123) | ŌĆō0.224 (ŌĆō0.598 to 0.231) | 0.139 (ŌĆō0.336 to 0.558) | ŌĆō0.159 (ŌĆō0.572 to 0.317) | 0.179 (ŌĆō0.299 to 0.585) |
| Camembert | NA | 0.423a) (ŌĆō0.012 to 0.723) | ŌĆō0.174 (ŌĆō0.564 to 0.280) | ŌĆō0.164 (ŌĆō0.575 to 0.313) | ŌĆō0.331 (ŌĆō0.682 to 0.145) | ŌĆō0.116 (ŌĆō0.541 to 0.357) |
| Eggs yolk | 0.098 (ŌĆō0.349 to 0.509) | ŌĆō0.048 (ŌĆō0.471 to 0.392) | ŌĆō0.094 (ŌĆō0.506 to 0.353) | 0.478a) (0.031 to 0.766) | 0.067 (ŌĆō0.399 to 0.505) | 0.232 (ŌĆō0.248 to 0.620) |
| Nuts | 0.084 (ŌĆō0.362 to 0.498) | NA | 0.202 (ŌĆō0.253 to 0.583) | 0.354 (ŌĆō0.119 to 0.696) | 0.379 (ŌĆō0.090 to 0.711) | 0.236 (ŌĆō0.244 to 0.623) |
References
1. Sun H, Gong TT, Jiang YT, Zhang S, Zhao YH, Wu QJ. Global, regional, and national prevalence and disability-adjusted life-years for infertility in 195 countries and territories, 1990-2017: results from a global burden of disease study, 2017. Aging (Albany NY) 2019;11:10952-91.



2. Agarwal A, Mulgund A, Hamada A, Chyatte MR. A unique view on male infertility around the globe. Reprod Biol Endocrinol 2015;13:37.




3. Fainberg J, Kashanian JA. Recent advances in understanding and managing male infertility. F1000Res 2019;8(F1000 Faculty Rev): 670.


4. Gosalvez J, Lopez-Fernandez C, Fernandez JL, Esteves SC, Johnston SD. Unpacking the mysteries of sperm DNA fragmentation: ten frequently asked questions. J Reprod Biotechnol Fertil 2015;4:2058915815594454.
5. Ebisch IM, Thomas CM, Peters WH, Braat DD, Steegers-Theunissen RP. The importance of folate, zinc and antioxidants in the pathogenesis and prevention of subfertility. Hum Reprod Update 2007;13:163-74.


6. Vujkovic M, Ocke MC, van der Spek PJ, Yazdanpanah N, Steegers EA, Steegers-Theunissen RP. Maternal Western dietary patterns and the risk of developing a cleft lip with or without a cleft palate. Obstet Gynecol 2007;110(2 Pt 1): 378-84.


7. Bassiri F, Tavalaee M, Dattilio M, Nasr-Esfahani MH. Micronutrients in support to the carbon cycle activate antioxidant defences and reduce sperm DNA damage in infertile men attending assisted reproductive technology programs: clinical trial study. Int J Fertil Steril 2020;14:57-62.


8. Forges T, Monnier-Barbarino P, Alberto JM, Gueant-Rodriguez RM, Daval JL, Gueant JL. Impact of folate and homocysteine metabolism on human reproductive health. Hum Reprod Update 2007;13:225-38.


10. Selhub J. Folate, vitamin B12 and vitamin B6 and one carbon metabolism. J Nutr Health Aging 2002;6:39-42.

12. Green R, Allen LH, Bjorke-Monsen AL, Brito A, Gueant JL, Miller JW, et al. Vitamin B12 deficiency. Nat Rev Dis Primers 2017;3:17040.



13. World Health Organization. WHO laboratory manual for the examination and processing of human semen. 5th ed. Geneva: World Health Organization; 2010.
14. Fernandez JL, Muriel L, Rivero MT, Goyanes V, Vazquez R, Alvarez JG. The sperm chromatin dispersion test: a simple method for the determination of sperm DNA fragmentation. J Androl 2003;24:59-66.


15. Fernandez JL, Muriel L, Goyanes V, Segrelles E, Gosalvez J, Enciso M, et al. Simple determination of human sperm DNA fragmentation with an improved sperm chromatin dispersion test. Fertil Steril 2005;84:833-42.


16. National Institute of Public Health (Instituto Nacional de Salud P├║blica). The epidemiological transition and the health system: TAHINA project. Results of the National Health Survey [Internet]. INSP. 2007;[cited 2023 Jan 14]. Available from: https://www.insp.dz/index.php/Non-categorise/enquetes.htmlf
17. Larson KL, DeJonge CJ, Barnes AM, Jost LK, Evenson DP. Sperm chromatin structure assay parameters as predictors of failed pregnancy following assisted reproductive techniques. Hum Reprod 2000;15:1717-22.


18. Velez de la Calle JF, Muller A, Walschaerts M, Clavere JL, Jimenez C, Wittemer C, et al. Sperm deoxyribonucleic acid fragmentation as assessed by the sperm chromatin dispersion test in assisted reproductive technology programs: results of a large prospective multicenter study. Fertil Steril 2008;90:1792-9.


19. Yuan HF, Zhao K, Zang Y, Liu CY, Hu ZY, Wei JJ, et al. Effect of folate deficiency on promoter methylation and gene expression of Esr1, Cav1, and Elavl1, and its influence on spermatogenesis. Oncotarget 2017;8:24130-41.



20. Hoek J, Steegers-Theunissen RP, Willemsen SP, Schoenmakers S. Paternal folate status and sperm quality, pregnancy outcomes, and epigenetics: a systematic review and meta-analysis. Mol Nutr Food Res 2020;64:e1900696.



21. Crha I, Kralikova M, Melounova J, Ventruba P, Zakova J, Beharka R, et al. Seminal plasma homocysteine, folate and cobalamin in men with obstructive and non-obstructive azoospermia. J Assist Reprod Genet 2010;27:533-8.




22. Wallock LM, Tamura T, Mayr CA, Johnston KE, Ames BN, Jacob RA. Low seminal plasma folate concentrations are associated with low sperm density and count in male smokers and nonsmokers. Fertil Steril 2001;75:252-9.


23. Boxmeer JC, Smit M, Utomo E, Romijn JC, Eijkemans MJ, Lindemans J, et al. Low folate in seminal plasma is associated with increased sperm DNA damage. Fertil Steril 2009;92:548-56.


24. Murphy LE, Mills JL, Molloy AM, Qian C, Carter TC, Strevens H, et al. Folate and vitamin B12 in idiopathic male infertility. Asian J Androl 2011;13:856-61.



25. Samavat J, Cantini G, Lorubbio M, DeglŌĆÖInnocenti S, Adaikalakoteswari A, Facchiano E, et al. Seminal but not serum levels of holotranscobalamin are altered in morbid obesity and correlate with semen quality: a pilot single centre study. Nutrients 2019;11:1540.



27. Terai K, Horie S, Fukuhara S, Miyagawa Y, Kobayashi K, Tsujimura A. Combination therapy with antioxidants improves total motile sperm counts: a preliminary study. Reprod Med Biol 2019;19:89-94.




28. Schisterman EF, Sjaarda LA, Clemons T, Carrell DT, Perkins NJ, Johnstone E, et al. Effect of folic acid and zinc supplementation in men on semen quality and live birth among couples undergoing infertility treatment: a randomized clinical trial. JAMA 2020;323:35-48.



29. Aarabi M, San Gabriel MC, Chan D, Behan NA, Caron M, Pastinen T, et al. High-dose folic acid supplementation alters the human sperm methylome and is influenced by the MTHFR C677T polymorphism. Hum Mol Genet 2015;24:6301-13.



30. Huang WJ, Lu XL, Li JT, Zhang JM. Effects of folic acid on oligozoospermia with MTHFR polymorphisms in term of seminal parameters, DNA fragmentation, and live birth rate: a double-blind, randomized, placebo-controlled trial. Andrology 2020;8:110-6.



31. Steiner AZ, Hansen KR, Barnhart KT, Cedars MI, Legro RS, Diamond MP, et al. The effect of antioxidants on male factor infertility: the Males, Antioxidants, and Infertility (MOXI) randomized clinical trial. Fertil Steril 2020;113:552-60.



32. Stenqvist A, Oleszczuk K, Leijonhufvud I, Giwercman A. Impact of antioxidant treatment on DNA fragmentation index: a double-blind placebo-controlled randomized trial. Andrology 2018;6:811-6.



33. Majzoub A, Agarwal A. Systematic review of antioxidant types and doses in male infertility: benefits on semen parameters, advanced sperm function, assisted reproduction and live-birth rate. Arab J Urol 2018;16:113-24.



34. Abad C, Amengual MJ, Gosalvez J, Coward K, Hannaoui N, Benet J, et al. Effects of oral antioxidant treatment upon the dynamics of human sperm DNA fragmentation and subpopulations of sperm with highly degraded DNA. Andrologia 2013;45:211-6.


35. Gual-Frau J, Abad C, Amengual MJ, Hannaoui N, Checa MA, Ribas-Maynou J, et al. Oral antioxidant treatment partly improves integrity of human sperm DNA in infertile grade I varicocele patients. Hum Fertil (Camb) 2015;18:225-9.


36. National Institute of Health; Office of Dietary Supplements. Folate: fact sheet for health professionals [Internet]. NIH. 2022;[cited 2023 Jan 14]. Available from: https://ods.od.nih.gov/factsheets/Folate-HealthProfessional/#en12
37. Wei MM, Gregory JF 3rd. Organic acids in selected foods inhibit intestinal brush border pteroylpolyglutamate hydrolase in vitro: potential mechanism affecting the bioavailability of dietary polyglutamyl folate. J Agric Food Chem 1998;46:211-9.


38. Watanabe F, Bito T. Vitamin B12 sources and microbial interaction. Exp Biol Med (Maywood) 2018;243:148-58.



39. Najafipour R, Moghbelinejad S, Aleyasin A, Jalilvand A. Effect of B9 and B12 vitamin intake on semen parameters and fertility of men with MTHFR polymorphisms. Andrology 2017;5:704-10.



40. Danielewicz A, Przybylowicz KE, Przybylowicz M. Dietary patterns and poor semen quality risk in men: a cross-sectional study. Nutrients 2018;10:1162.



41. Jurewicz J, Radwan M, Sobala W, Radwan P, Bochenek M, Hanke W. Dietary patterns and their relationship with semen quality. Am J Mens Health 2018;12:575-83.



42. Salas-Huetos A, Bullo M, Salas-Salvado J. Dietary patterns, foods and nutrients in male fertility parameters and fecundability: a systematic review of observational studies. Hum Reprod Update 2017;23:371-89.


43. Liu CY, Chou YC, Chao JC, Hsu CY, Cha TL, Tsao CW. The association between dietary patterns and semen quality in a general asian population of 7282 males. PLoS One 2015;10:e0134224.



44. Eslamian G, Amirjannati N, Rashidkhani B, Sadeghi MR, Hekmatdoost A. Nutrient patterns and asthenozoospermia: a case-control study. Andrologia 2017;49:e12624.


45. Chiu YH, Afeiche MC, Gaskins AJ, Williams PL, Petrozza JC, Tanrikut C, et al. Fruit and vegetable intake and their pesticide residues in relation to semen quality among men from a fertility clinic. Hum Reprod 2015;30:1342-51.



46. Mebdoua S, Lazali M, Ounane SM, Tellah S, Nabi F, Ounane G. Evaluation of pesticide residues in fruits and vegetables from Algeria. Food Addit Contam Part B Surveill 2017;10:91-8.


47. Nassan FL, Chavarro JE, Tanrikut C. Diet and menŌĆÖs fertility: does diet affect sperm quality? Fertil Steril 2018;110:570-7.


48. Afeiche MC, Williams PL, Gaskins AJ, Mendiola J, Jorgensen N, Swan SH, et al. Meat intake and reproductive parameters among young men. Epidemiology 2014;25:323-30.



49. Silbernagel SM, Carpenter DO, Gilbert SG, Gochfeld M, Groth E 3rd, Hightower JM, et al. Recognizing and preventing overexposure to methylmercury from fish and seafood consumption: information for physicians. J Toxicol 2011;2011:983072.




50. M├Łnguez-Alarcon L, Afeiche MC, Williams PL, Arvizu M, Tanrikut C, Amarasiriwardena CJ, et al. Hair mercury (Hg) levels, fish consumption and semen parameters among men attending a fertility center. Int J Hyg Environ Health 2018;221:174-82.


- TOOLS







