|
 |
- Search
| Clin Exp Reprod Med > Volume 42(4); 2015 > Article |
Abstract
Objective
Smoking has been reported to harm nearly every organ of the body, but conflicting results have been reported regarding the effects of smoking on assisted conception. In this prospective cohort study, we aimed to investigate the prevalence of positive urinary cotinine tests in infertile couples and whether cotinine positivity was associated with infertility treatment outcomes.
Methods
A qualitative urinary cotinine test was administered to 127 couples who underwent in vitro fertilization (IVF, n=92) or intrauterine insemination (IUI, n=35).
Results
The overall prevalence of positive urinary cotinine test was 43.3% (55/127) in the male partners and 10.2% (13/127) in the female partners with similar prevalence rates in both genders in the IUI and IVF groups. Semen characteristics, serum markers of ovarian reserve, and number of retrieved oocytes were comparable among cotinine-positive and cotinine-negative men or women (with the exception of sperm count, which was higher among cotinine-positive men). The results of urinary cotinine tests in infertile couples were not associated with IVF and IUI outcomes.
Smoking has been reported to harm nearly every organ of the body and has been found to impair natural and assisted fecundity [1,2,3]. In women, smoking is associated with decreased rates of fertilization and pregnancy [4,5,6,7], and has been found to reduce natural and in vitro fertilization (IVF) conception rate by up to approximately 34% to 46% [1,3,8]. However, some studies have reported smoking in women had no detrimental effect on fertilization and IVF pregnancy rates [3,9,10].
In male smokers, smoking has been demonstrated to result in reduction in multiple sperm parameters has been demonstrated [3,11,12,13] but other studies found smoking to have no harmful effects on fertility [14,15]. Male smoking status was not found to affect pregnancy rates in IVF cycles [3] and a recent report also demonstrated that smoking, as measured by seminal plasma cotinine, was not associated with detrimental effects on IVF outcomes [16]. Overall, the effects of smoking on assisted conception have not been securely established, and many conflicting results have been reported.
The Korea National Health and Nutrition Examination Survey (KNHANES) conducted from 2007 to 2009 found that the overall prevalence of smoking in Korea was still relatively high, at 47.4% in men and 6.8% in women [17]. However, self-reported smoking has been suggested to be an unreliable metric [18,19]. Female smokers may experience considerable social and medical pressure to quit smoking and it is especially likely for women who smoke not to report their smoking status accurately. Thus, a more objective method for assessing smoking status determination is necessary. Several such metrics have been validated, of which the measurement of cotinine, a nicotine metabolite, is the most widely used [20].
No previous reports have evaluated the prevalence of smoking in infertile couples in Korea and its effect on the outcomes of infertility treatment. This study aimed to investigate the prevalence of positive urinary cotinine tests in infertile couples and to determine whether smoking, as measured by cotinine positivity, affected infertility treatment outcomes.
In the present study, qualitative urinary cotinine test was used as an objective measurement of smoking status, regardless of self-reported past, current or passive smoking. Urinary cotinine was tested in 127 couples who underwent IVF (n=92) or intrauterine insemination (IUI) (n=35) between 2012 and 2014. A qualitative urinary cotinine test (positive or negative) was performed with a commercial kit (Nico-Find; Humasis, Anyang, Korea) on the day of oocyte retrieval or on the day of IUI. The cutoff concentration of urinary cotinine kit for a positive result was 200 ng/mL, and the sensitivity and specificity of the urinary cotinine test kit were 100% and 94%, respectively. Only one IVF or IUI cycle per couple was included and the clinical outcomes of each couple were prospectively followed.
In female participants, body mass index, and basal serum levels of follicle-stimulating hormone (FSH) and anti-Müllerian hormone (AMH) were analyzed in the present study if they were measured within 3 months of the artificial conception cycle. Ovarian stimulation for IVF was started on the second or third day of the cycle, using recombinant FSH (Gonal-F, Serono, Geneva, Switzerland) with or without highly purified human menopausal gonadotropin (hMG) (Menopur, Ferring, Malmo, Sweden). Pituitary suppression was performed using a gonadotropin-releasing hormone (GnRH) agonist (Decapeptyl 0.1 mg/day; Ferring) or antagonist (Cetrotide 0.25 mg/day; Serono). Ovulation was triggered by recombinant human chorionic gonadotropin (hCG) (Ovidrel, Serono) when either the leading follicle reached a mean diameter of 18 mm or two or more follicles reached a diameter of 17 mm. Oocytes were retrieved under transvaginal ultrasound guidance 34 to 36 hours after the administration of recombinant hCG. Other IVF procedures were performed as described elsewhere [21].
After fertilization, all embryos were evaluated for cell number, degree of fragmentation, and cell size. Three days after oocyte retrieval, embryos were classified from grade A to D with grade A embryos considered to be high-quality. The embryos were selected for transfer using standard laboratory procedures, according to embryo morphology on day 3 or blastocyst morphology on day 5. Blastocysts were evaluated based on the number of evenly sized cells, the amount of visible inner cell mass and the presence of a continuous trophectoderm with sufficient cells. Up to three embryos were transferred 3 days after oocyte retrieval or up to two blastocysts were transferred 5 days after oocyte retrieval. The luteal phase was supported with 50 mg of intramuscular progesterone in oil (Progesterone, Genefer, Seoul, Korea) daily, starting on the day of oocyte retrieval. If an intrauterine pregnancy was identified, progesterone was continued for another 5 weeks. Pregnancy was first assessed by serum β-hCG 14 days after oocyte retrieval and a clinical pregnancy was defined as the presence of visible fetal cardiac activity.
The IUI was performed according to previously published methods [22]. Ovarian stimulation was performed by recombinant FSH alone, clomiphene with recombinant FSH, or a natural cycle. Semen was collected by masturbation at the time of IUI or oocyte retrieval and evaluated by using computer-assisted semen analysis (SAIS-Plus 10.1, Medical Supply Co., Wonju, Korea) within 1 hour of collection. The following semen parameters were evaluated: volume (mL), sperm concentration (106/mL), motility (% progressive), and total motile sperm count (volume×sperm concentration×percent of motility/100). Sperm morphology was assessed using strict criteria. Sperm DNA fragmentation was measured using terminal deoxynucleotidyl transferase-mediated dUDP nick-end labelling (TUNEL) method [23].
All statistical analyses were performed using SPSS ver. 18.0 (SPSS Inc., Chicago, IL, USA). All data were presented as mean±standard deviation. The chi-square test was used to compare frequencies but Fisher's exact test was applied if the expected cell number was less than five. The Mann-Whitney U test was used to compare mean values between two groups, while the Kruskal-Wallis test was used to compare mean values among three groups. Pearson correlation coefficient was used to evaluate the extent to which the smoking status of one partner in a couple was correlated that of the other partner. Two-tailed p-values <0.05 were considered to indicate statistical significance.
All participants provided written informed consent, and the Institutional Review Board of Seoul National University Bundang Hospital approved the study protocol (IRB no. B-1210-176-002).
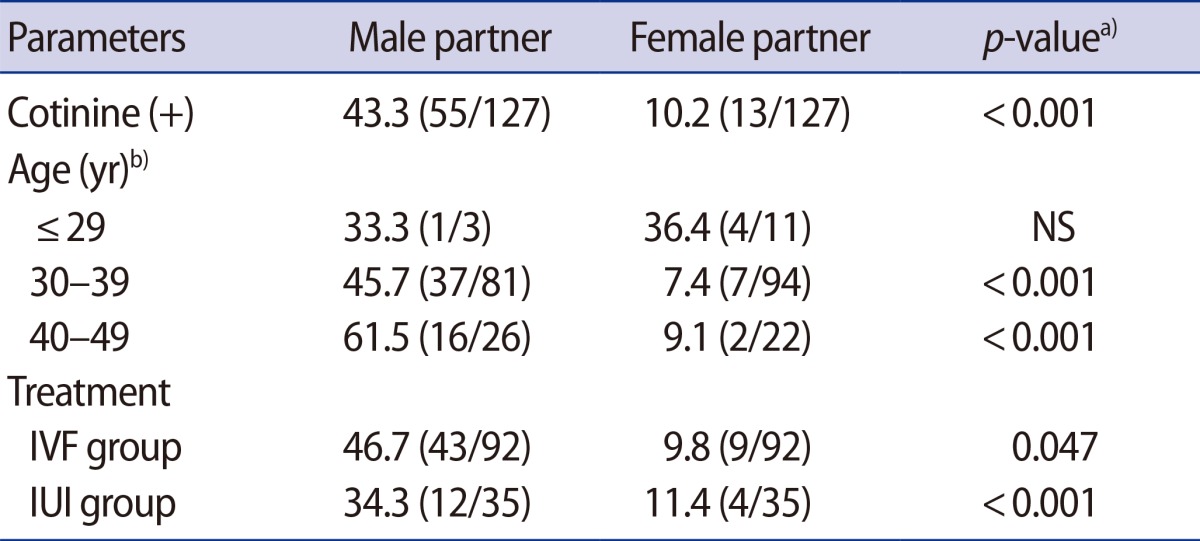
The overall prevalence of positive urinary cotinine test was much higher in male participants (43.3%, 55/127) than in female participants (10.2%, 13/127) and this finding did not vary significantly based on treatment method or age (Table 1). The highest prevalence was observed in men between 40 and 50 years of age and women between 20 and 30 years of age. The prevalence was similar in the IUI and IVF group: 34.3% (12/35) vs. 46.7% (43/92), respectively in the male participants and 11.4% (4/35) vs. 9.8% (9/92), respectively in the female participants.
Positive urinary cotinine tests in both male and female partners were observed in 7.9% of all couples and in 54.3% of couples, both partners had negative results. This tendency was statistically significant (r=0.229, p=0.01) (Table 2). Table 3 presents semen characteristics according to urinary cotinine positivity in all male participants. With the exception of sperm count, no semen parameters showed significant variance according to cotinine-positivity.
Among the female participants, cotinine-positive participants was younger than cotinine-negative women (mean age, 32.4±5.3 years vs. 35.1±4.6 years; p=0.026), but the causes of infertility, body mass index (21.5±2.4 kg/m2 vs. 22.3±3.7 kg/m2), basal level of serum FSH (5.8±1.2 IU/L vs. 6.4±3.1 IU/L) and AMH (3.4±2.9 ng/mL vs. 2.4±2.0 ng/mL) of cotinine-positive women (n=13) were comparable to those of cotinine-negative women (n=114) (Table 4). In IVF cycles (n=92), the number of cotinine-positive women was small (n=9), but age, the cause of infertility, body mass index, and basal serum FSH and AMH levels were similar among cotinine-positive and cotinine-negative subjects. The number of oocytes retrieved was also similar (8.9±5.5 vs. 7.3±7.2). Cycles with no mature oocyte were absent in cotinine-positive women but such cycles were noted in two cotinine-negative women (data not shown). In 92 IVF cycles, a negative urinary cotinine test in both partners was observed in 49 couples. A positive test in the male partner but a negative test in the female partner was observed in 34 couples. In nine couples, both partners had positive urinary cotinine tests. No couples were observed in which the male partner had a negative result and the female partner had a positive result. In Table 4, IVF outcomes according to cotinine test results are presented and no parameters were found to vary significantly depending on cotinine co-positivity status.
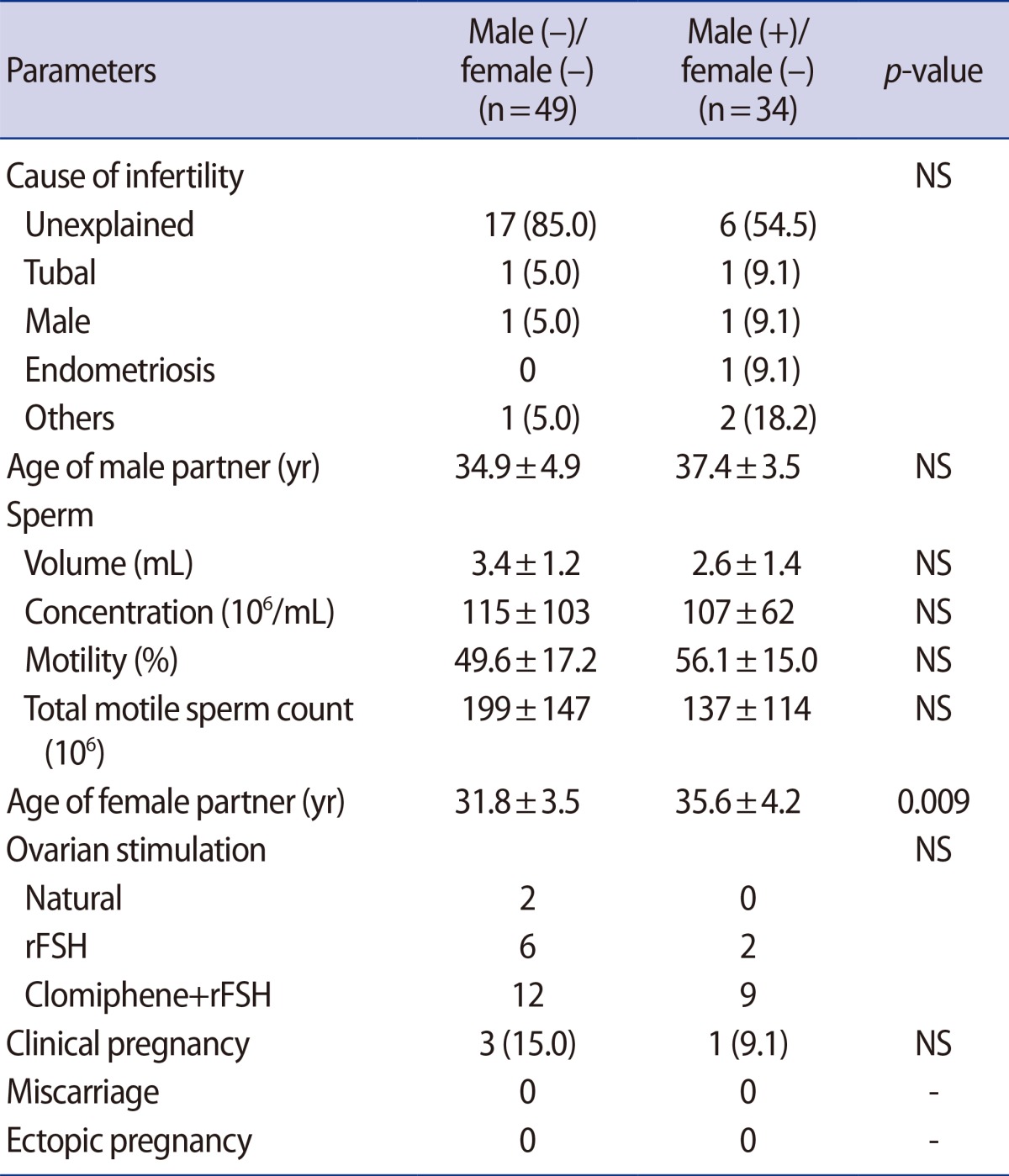
In 35 IUI cycles, both partners had a negative urinary cotinine test in 20 couples, and 11 male-positive couples were identified (Table 5). Male-negative and female-positive results were observed in three couples and in one couple, both partners were positive. When IUI outcomes were compared between the both-negative and male-positive/female-negative groups, no parameters were found to be significant except the age of the female participants.
In the present study, the prevalence of positive urinary test was 43.3% in male participants and 10.2% in female participants, which is comparable to the smoking prevalence derived from the fourth KNHANES, a nationwide representative survey conducted by the Korean Ministry of Health and Welfare from 2007 to 2009 (42.1% and 7.3% in reproductive-age men and women, respectively) [17,24]. Smoking rates still appear to be relatively high despite recent campaigns to reduce smoking in Korea.
Since cigarette smoke contains well-known harmful substances, concerns have been raised about the potential adverse effects of smoking on male fertility [25]. Although several studies have reported a modest reduction in the semen parameters of smokers compared to non-smokers, other studies have not demonstrated a reduction in male fertility associated with smoking [26,27,28,29,30,31,32]. Similarly, this study found no significant differences in sperm characteristics depending on the results of urinary cotinine test, and the concentration of sperm was in fact higher in cotinine-positive men than in cotininemen. The reasons for considerable discrepancies that exist among studies are still unclear, although several methodological issues can be suggested. Regarding the determination of sperm quality, considerable variation might exist among different laboratories despite newly changed World Health Organization reference values for human semen characteristics [33]. Additionally, sperm quality can be affected by local environmental elements, including stress, the amount of nicotine in the tobacco that is consumed, and other life-style factors. Additionally, men with erectile dysfunction which is associated with smoking might refuse to participate in such studies and this potential selection bias could affect the results of the studies.
In the present study, we did not find any significant negative effects of cigarette smoking, as documented by urinary cotinine on IVF outcomes, which partially corresponds to the findings of a recent report by Cinar et al. [16]. The fact that assisted reproduction technology (ART) allows the opportunity to select high-quality embryos [10] may explain why the outcomes of fertility treatment were similar in smokers and non-smokers.
Additionally, the number of retrieved oocytes and serum levels of ovarian reserve markers were similar among cotinine-positive and cotinine-negative women indicating that the presence of cotinine was not associated with diminished ovarian reserve. In the present study, the rate of cotinine positivity was significantly higher in women younger than 30 years of age, and the detrimental effect of smoking might have been counteracted by the higher fertility of the younger participants. This is partially in accordance with reports that have found that the harmful effect of smoking are more distinct in elderly women undergoing ART treatment [2,14,34,35]. Moreover, the Practice Committee of the American Society for Reproductive Medicine has also stated that the effects of smoking and old age might have a synergistic effect on the acceleration of oocyte depletion [36]. Therefore, stratification according to age groups is needed in further studies with larger study populations.
To the best of our knowledge, this is the first study to evaluate the association between objectively determined smoking status and the outcomes of fertility treatment in Korean population. Moreover, a major strength of the present study is that urinary cotinine co-positivity in couple was assessed. Urinary cotinine was used as an objective indicator of smoking and the participants were not asked whether they smoked. In a previous study performed in Korean population, the self-reported prevalence of smoking in men was 47.8%, compared to a cotinine-verified smoking rate was 52.2%, whereas among women, the self-reported smoking rate was 6.6%, while the cotinine positivity rate was 14.5% [37]. Therefore, self-reported smoking status may not agree with tests of biomarkers of tobacco use, and this discrepancy may be larger in women because female smokers are still stigmatized in Asian societies. The self-reported smoking rates in other ethnic populations also underestimate the actual prevalence of cigarette smoking by up to 4% [38,39]. In this study, qualitative urinary cotinine results (positive or negative) were used to objectively assess participants' smoking status meaning that it was not possible to evaluate the relationship urinary cotinine levels with smoking frequency, semen parameters, ovarian reserve, and the outcomes of ART treatment.
Cotinine is the major metabolite of nicotine and 75% of nicotine is converted to cotinine in human. Cotinine is easily detectable in body fluids and is widely accepted as a biomarker of cigarette smoke exposure due to its specificity and relatively long half-life in the body (16 hours) compared to nicotine (2 hours) [40]. The urinary cotinine kit used in this study had a cutoff value for a positive result of 200 ng/mL and the sensitivity of this commercial kit was relatively high (96%). Since the half-life of cotinine is approximately 16 hours [40], a heavy smoker who abstains from tobacco for several days may demonstrate an undetectable urinary cotinine level, leading to an inappropriate classification as cotinine-negative. Furthermore, less intense and less frequent smokers can demonstrate urinary cotinine-negativity; therefore, a highly sensitive test is needed to minimize the misclassification of true smokers as nonsmokers. Recently, several studies have found appropriate cotinine cutoff values to vary according to race and ethnicity [40,41] and the optimal cutoff value for urinary cotinine levels has been suggested to be 164 ng/mL in a study of the Korean population [42].
This study had some limitations. First, only urinary cotinine was measured as a biomarker for smoking in the present study. In addition to cotinine, other alkaloids including anabasine and nornicotine can be used as unique markers for smoking, however, these markers do not reflect passive exposure to smoking. Moreover, cotinine has been validated as a monitoring tool for smoking in numerous studies [19,20,43]. Second, this study included a relatively small number of participants undergoing ART. The small study population may have decreased the power of the study, meaning that the findings of the present study may have been due to chance and should be interpreted with caution. Thus, a much larger study population with age stratification may be required to achieve sufficient statistical power to adequately assess the relationship between smoking and ART outcomes. Finally, light smokers may have been inappropriately classified in the present study because the concentration of urinary cotinine in light smokers or moderate passive smokers has been reported to be lower than the threshold used in the present study [41]. Also, urinary cotinine test may demonstrate positive results in nicotine patch or gum users and may not reflect past smoking history. In general, due to these considerations, urinary cotinine test is used only for screening test in healthcare examination, not for medical purposes. Gas chromatography is the preferable quantitative assay for cotinine, and a questionnaire could potentially be considered as an alternative to urinary cotinine test. However, questionnaires are not objective and it is unlikely that all study participants would have answered the questionnaire honestly. Urinary cotinine tests were therefore used in the present study despite the fact that positive urinary cotinine test do not correlate perfectly with smoking.
In conclusion, positive urinary cotinine test was not associated with negative impact on infertility treatment outcomes. Further prospective studies are needed with larger populations in order to elucidate the association between smoking and infertility.
Notes
References
1. Augood C, Duckitt K, Templeton AA. Smoking and female infertility: a systematic review and meta-analysis. Hum Reprod 1998;13:1532-1539.PMID: 9688387.



2. Hughes EG, Brennan BG. Does cigarette smoking impair natural or assisted fecundity? Fertil Steril 1996;66:679-689.PMID: 8893667.


3. Hughes EG, Yeo J, Claman P, YoungLai EV, Sagle MA, Daya S, et al. Cigarette smoking and the outcomes of in vitro fertilization: measurement of effect size and levels of action. Fertil Steril 1994;62:807-814.PMID: 7926092.


4. Crha I, Hruba D, Fiala J, Ventruba P, Zakova J, Petrenko M. The outcome of infertility treatment by in-vitro fertilisation in smoking and non-smoking women. Cent Eur J Public Health 2001;9:64-68.PMID: 11503276.

5. Gruber I, Just A, Birner M, Losch A. Effect of a woman's smoking status on oocyte, zygote, and day 3 pre-embryo quality in in vitro fertilization and embryo transfer program. Fertil Steril 2008;90:1249-1252.PMID: 17905237.


6. Klonoff-Cohen H, Natarajan L, Marrs R, Yee B. Effects of female and male smoking on success rates of IVF and gamete intra-Fallopian transfer. Hum Reprod 2001;16:1382-1390.PMID: 11425817.



7. Neal MS, Hughes EG, Holloway AC, Foster WG. Sidestream smoking is equally as damaging as mainstream smoking on IVF outcomes. Hum Reprod 2005;20:2531-2535.PMID: 15919779.



8. Waylen AL, Metwally M, Jones GL, Wilkinson AJ, Ledger WL. Effects of cigarette smoking upon clinical outcomes of assisted reproduction: a meta-analysis. Hum Reprod Update 2009;15:31-44.PMID: 18927070.



9. Sterzik K, Strehler E, De Santo M, Trumpp N, Abt M, Rosenbusch B, et al. Influence of smoking on fertility in women attending an in vitro fertilization program. Fertil Steril 1996;65:810-814.PMID: 8654644.


10. Wright KP, Trimarchi JR, Allsworth J, Keefe D. The effect of female tobacco smoking on IVF outcomes. Hum Reprod 2006;21:2930-2934.PMID: 16840799.



11. Pasqualotto FF, Umezu FM, Salvador M, Borges E Jr, Sobreiro BP, Pasqualotto EB. Effect of cigarette smoking on antioxidant levels and presence of leukocytospermia in infertile men: a prospective study. Fertil Steril 2008;90:278-283.PMID: 18462724.


12. Said TM, Ranga G, Agarwal A. Relationship between semen quality and tobacco chewing in men undergoing infertility evaluation. Fertil Steril 2005;84:649-653.PMID: 16169398.


13. Sofikitis N, Miyagawa I, Dimitriadis D, Zavos P, Sikka S, Hellstrom W. Effects of smoking on testicular function, semen quality and sperm fertilizing capacity. J Urol 1995;154:1030-1034.PMID: 7637048.


14. Joesbury KA, Edirisinghe WR, Phillips MR, Yovich JL. Evidence that male smoking affects the likelihood of a pregnancy following IVF treatment: application of the modified cumulative embryo score. Hum Reprod 1998;13:1506-1513.PMID: 9688383.



16. Cinar O, Dilbaz S, Terzioglu F, Karahalil B, Yucel C, Turk R, et al. Does cigarette smoking really have detrimental effects on outcomes of IVF? Eur J Obstet Gynecol Reprod Biol 2014;174:106-110.PMID: 24424210.


17. Kim SE, Shim JH, Noh H, Hwang HS, Park HK. The relationship between smoking status and suicidal behavior in Korean adults: the 4th Korea National Health and Nutrition Examination Survey (2007-2009). Korean J Fam Med 2013;34:178-189.PMID: 23730485.



18. Patrick DL, Cheadle A, Thompson DC, Diehr P, Koepsell T, Kinne S. The validity of self-reported smoking: a review and meta-analysis. Am J Public Health 1994;84:1086-1093.PMID: 8017530.



19. Tunstall-Pedoe H, Woodward M, Brown CA. The drinking, passive smoking, smoking deception and serum cotinine in the Scottish Heart Health Study. J Clin Epidemiol 1991;44:1411-1414.PMID: 1753272.


20. Jones-Burton C, Vessal G, Brown J, Dowling TC, Fink JC. Urinary cotinine as an objective measure of cigarette smoking in chronic kidney disease. Nephrol Dial Transplant 2007;22:1950-1954.PMID: 17369616.



21. Lee JE, Lee JR, Jee BC, Suh CS, Kim KC, Lee WD, et al. Clinical application of anti-Mullerian hormone as a predictor of controlled ovarian hyperstimulation outcome. Clin Exp Reprod Med 2012;39:176-181.PMID: 23346529.



22. Yi G, Jee BC, Suh CS, Kim SH. Stimulated intrauterine insemination in women with unilateral tubal occlusion. Clin Exp Reprod Med 2012;39:68-72.PMID: 22816072.



23. Jee BC, Suh CS, Shin MS, Lee HJ, Lee JH, Kim SH. Sperm nuclear DNA fragmentation and chromatin structure in one-day-old ejaculated sperm. Clin Exp Reprod Med 2011;38:82-86.PMID: 22384423.



24. Lee JY, Ko YJ, Park SM. Factors associated with current smoking and heavy alcohol consumption among women of reproductive age: the Fourth Korean National Health and Nutrition Examination Survey 2007-2009. Public Health 2013;127:473-481.PMID: 23608023.


26. de Mouzon J, Spira A, Schwartz D. A prospective study of the relation between smoking and fertility. Int J Epidemiol 1988;17:378-384.PMID: 3403134.



27. Dikshit RK, Buch JG, Mansuri SM. Effect of tobacco consumption on semen quality of a population of hypofertile males. Fertil Steril 1987;48:334-336.PMID: 3609347.


28. Dunphy BC, Barratt CL, von Tongelen BP, Cooke ID. Male cigarette smoking and fecundity in couples attending an infertility clinic. Andrologia 1991;23:223-225.PMID: 1741486.


29. Goverde HJ, Dekker HS, Janssen HJ, Bastiaans BA, Rolland R, Zielhuis GA. Semen quality and frequency of smoking and alcohol consumption: an explorative study. Int J Fertil Menopausal Stud 1995;40:135-138.PMID: 7663540.

30. Oldereid NB, Rui H, Clausen OP, Purvis K. Cigarette smoking and human sperm quality assessed by laser-Doppler spectroscopy and DNA flow cytometry. J Reprod Fertil 1989;86:731-736.PMID: 2760898.


31. Oldereid NB, Rui H, Purvis K. Lifestyles of men in barren couples and their relationships to sperm quality. Eur J Obstet Gynecol Reprod Biol 1992;43:51-57.PMID: 1737609.


32. Osser S, Beckman-Ramirez A, Liedholm P. Semen quality of smoking and non-smoking men in infertile couples in a Swedish population. Acta Obstet Gynecol Scand 1992;71:215-218.PMID: 1317645.


33. Cooper TG, Noonan E, von Eckardstein S, Auger J, Baker HW, Behre HM, et al. World Health Organization reference values for human semen characteristics. Hum Reprod Update 2010;16:231-245.PMID: 19934213.



34. Sharara FI, Beatse SN, Leonardi MR, Navot D, Scott RT Jr. Cigarette smoking accelerates the development of diminished ovarian reserve as evidenced by the clomiphene citrate challenge test. Fertil Steril 1994;62:257-262.PMID: 8034069.


35. Zenzes MT, Reed TE, Casper RF. Effects of cigarette smoking and age on the maturation of human oocytes. Hum Reprod 1997;12:1736-1741.PMID: 9308804.



36. Practice Committee of the American Society for Reproductive Medicine. Smoking and infertility: a committee opinion. Fertil Steril 2012;98:1400-1406.PMID: 22959451.


37. Kang HG, Kwon KH, Lee IW, Jung B, Park EC, Jang SI. Biochemically-verified smoking rate trends and factors associated with inaccurate self-reporting of smoking habits in Korean women. Asian Pac J Cancer Prev 2013;14:6807-6812.PMID: 24377610.



38. Caraballo RS, Giovino GA, Pechacek TF, Mowery PD. Factors associated with discrepancies between self-reports on cigarette smoking and measured serum cotinine levels among persons aged 17 years or older: Third National Health and Nutrition Examination Survey, 1988-1994. Am J Epidemiol 2001;153:807-814.PMID: 11296155.



39. Perez-Stable EJ, Marin G, Marin BV, Benowitz NL. Misclassification of smoking status by self-reported cigarette consumption. Am Rev Respir Dis 1992;145:53-57.PMID: 1731599.


40. Benowitz NL, Hukkanen J, Jacob P 3rd. Nicotine chemistry, metabolism, kinetics and biomarkers. In: Henningfield JE, London ED, Pogun S, editors. Nicotine psychopharmacology. Berlin: Springer; 2009. p. 29-60.
41. Jarvis MJ, Fidler J, Mindell J, Feyerabend C, West R. Assessing smoking status in children, adolescents and adults: cotinine cutpoints revisited. Addiction 2008;103:1553-1561.PMID: 18783507.


42. Kim S, Jung A. Optimum cutoff value of urinary cotinine distinguishing South Korean adult smokers from nonsmokers using data from the KNHANES (2008-2010). Nicotine Tob Res 2013;15:1608-1616.PMID: 23509092.



43. Hald J, Overgaard J, Grau C. Evaluation of objective measures of smoking status: a prospective clinical study in a group of head and neck cancer patients treated with radiotherapy. Acta Oncol 2003;42:154-159.PMID: 12801134.


Table 4
In vitro fertilization outcomes according to cotinine positivity in male and female partner
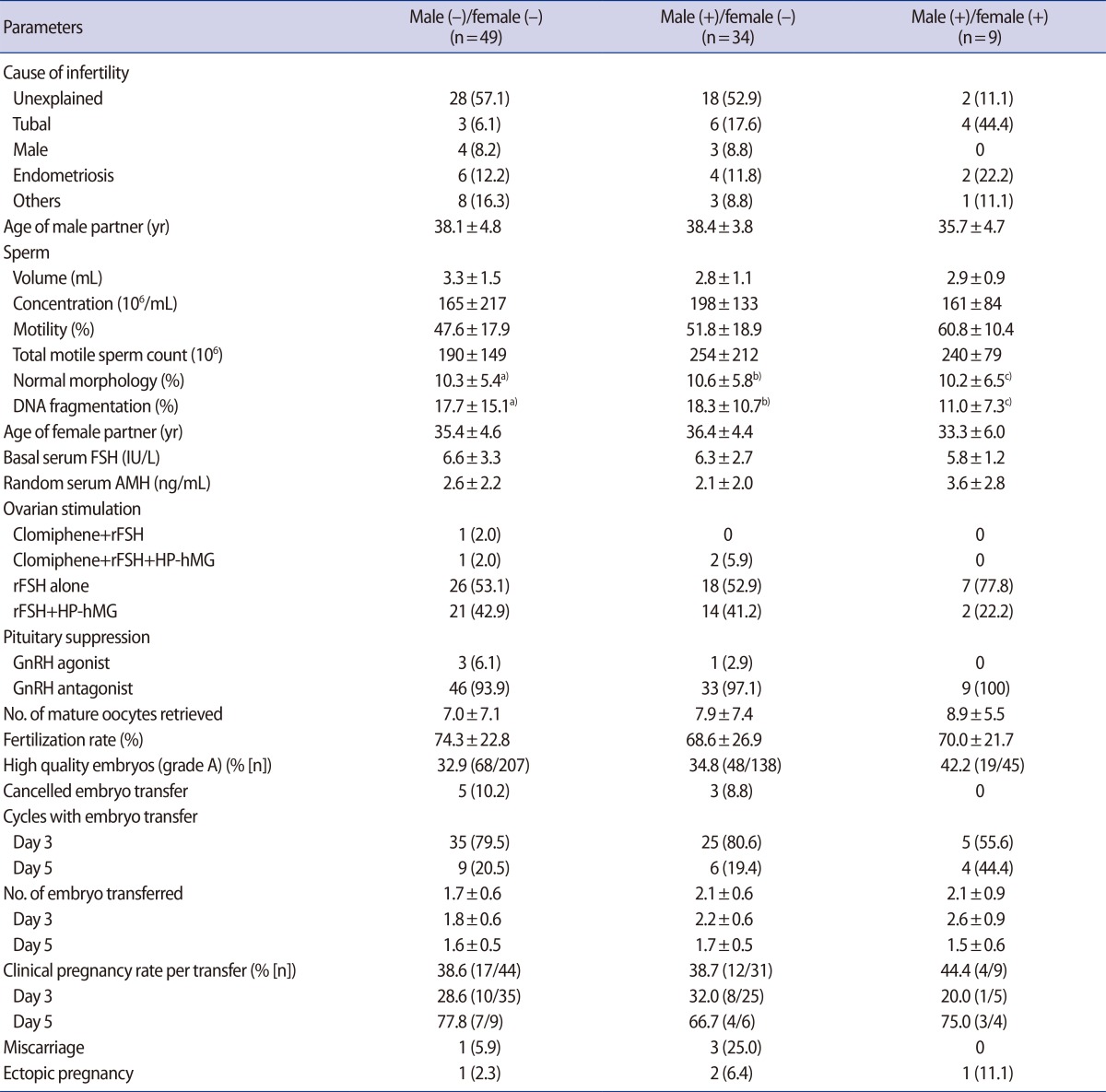
Values are presented as number (%) or mean±standard deviation unless otherwise indicated. No parameters were significantly different among the three groups.
FSH, follicle-stimulating hormone; AMH, anti-Müllerian hormone; rFSH, recombinant FSH; HP-hMG, highly purified human menopausal gonadotropin; GnRH, gonadotropin-releasing hormone.
a)n=30; b)n=20; c)n=7.