Preferred strategy for euploid single embryo transfer in advanced maternal age: Fresh versus frozen
Article information
Abstract
Objective
The purpose of this study was to compare fresh and frozen-thawed euploid blastocyst transfer protocols following preimplantation genetic screening (PGS) in cases of advanced maternal age.
Methods
A total of 330 patients were examined retrospectively. PGS was performed on the embryos of 146 patients for whom fresh transfers were chosen. In contrast, frozen-thawed euploid single embryo transfer (ET) was selected after PGS for 184 patients, and their embryos were vitrified. The percentage of euploid embryos and rates of implantation, pregnancy, and pregnancy continuity, as well as clinical and biochemical abortion rates, were compared.
Results
The numbers of retrieved oocytes, metaphase II oocytes, and fertilized ova were greater in the frozen-thawed group. The percentages of euploid embryos were comparable between the fresh and frozen-thawed groups (32% vs. 34.8%, respectively). The rates of implantation (46.6%vs. 62.5%), pregnancy (50% vs. 66.8%), ongoing pregnancy (38.4% vs. 53.8%), and live birth percentage (37.0% vs. 53.8%) were significantly higher in the frozen-thawed group. However, no significant differences were found in the clinical and biochemical abortion rates.
Conclusion
The use of frozen-thawed single euploid ET is associated with increased implantation and pregnancy rates compared to fresh single euploid ET with PGS.
Introduction
Advanced maternal age (AMA) is associated with decreased implantation rates, increased miscarriage rates, and fetal chromosomal abnormalities [1]. The primary factor impairing the success of assisted reproductive technology (ART) is the presence of aneuploid embryos, which is dependent on maternal age [2].
Preimplantation genetic screening (PGS) presents a viable option that can reduce abortion rates and shorten the time to achieve live birth in AMA patients undergoing ART [3,4]. At present, trophectoderm (TE) biopsy at the blastocyst stage has the potential to become the gold-standard technique for PGS [5,6]. Moreover, incorporating TE biopsy for PGS into the conventional morphological parameters involved in embryo quality assessment may improve pregnancy outcomes in AMA patients, while also reducing recurrent implantation failures and spontaneous abortion [6].
Recent advancements in cryopreservation methods offer an opportunity to postpone embryo transfer (ET), thereby avoiding the non-physiological endometrium that exists during controlled ovarian hyperstimulation (COH). This has led to improvements in implantation rates and pregnancy outcomes [7]. Since delayed ET may facilitate a more receptive endometrium in the subsequent cycle, it could serve to mitigate the negative effects of COH, as suboptimal endometrial development can reduce the likelihood of embryo implantation and result in lower pregnancy rates [8]. Furthermore, frozen-thawed ET allows for the inclusion of an entire cohort of embryos, including those from the fifth and sixth days after fertilization. In contrast, slower-growing embryos may be biopsied on day 5 or day 6 during fresh ET with PGS, which could negatively impact the cohort of embryos available for transfer [9].
PGS also enhances the implantation potential and live birth rates associated with euploid embryos in AMA patients [10]. PGS presents a feasible solution that may reduce abortion rates and shorten the time to achieve live birth in AMA patients undergoing ART. At present, two distinct transfer strategies, involving either fresh or frozen-thawed embryos, are employed in clinical practice [9]. A frozen ET strategy has recently been suggested to improve pregnancy rates due to enhanced endometrial receptivity [8]. However, the outcomes of the ET strategy for euploid embryos require further investigation in AMA patients. In this study, we compared the transfers of single fresh and frozen-thawed euploid blastocysts after PGS with TE biopsy in the context of AMA.
Methods
This study was structured as a single-center cohort investigation. We retrospectively examined patients who underwent ET in the ART and Reproductive Genetics Center of Istanbul Memorial Hospital between the years 2011 and 2020. The Erzincan University Ethics Committee granted approval for this research (2019-12). The study was conducted in compliance with guidelines equivalent to those of an Institutional Review Board, in accordance with the Declaration of Helsinki. Informed consent was secured from each participant included in the study.
1. Patient selection
The study included a total of 330 AMA patients between the ages of 38 and 43 years. Of these, 146 patients underwent single euploid ET with fresh blastocysts, while 184 patients underwent single euploid ET with frozen-thawed embryos. All patients underwent ET on either day 5 or day 6, accompanied by TE biopsy. The rates of embryo implantation, abortion, and live birth in fresh and frozen-thawed ETs with PGS were compared between the groups.
The exclusion criteria were defined as follows: progesterone levels exceeding 1.5 ng/mL at the trigger point, fresh and frozen-thawed ETs not conducted exclusively with good-quality embryos (characterized by six to 10 cells with 20% fragmentation and uniform blastomere size), preimplantation genetic diagnosis of a single-gene or chromosomal disorder, egg donor cycles, gender selection cycles, any medical or surgical intervention involving the fallopian tubes or uterus, and severe male factor infertility requiring surgical sperm retrieval. If estradiol levels exceeded 3,000 IU on the trigger day in a fresh cycle, a freeze-all strategy was preferred, and fresh ET was not considered.
2. Study protocol
Gonadotropin-releasing hormone antagonist protocols were followed, and exogenous gonadotropins, including recombinant follicle-stimulating hormone (Gonal-f; Merck Serono) and human menopausal gonadotropin (Menogon; Merck Serono), were employed for COH. The treatment commenced on the 2nd or 3rd day of the cycle, with drug dosages ranging from 150 to 450 IU daily. When the leading follicle attained a size of 14 mm, a gonadotropin-releasing hormone antagonist (cetrorelix, Cetrotide; Merck Serono) was administered to suppress the pituitary gland. To ensure the final maturation of the oocyte, an intramuscular injection of 6,000 IU human chorionic gonadotropin (hCG, Ovitrelle 0.5 mL; Merck Serono) was given once the follicle diameter reached 17 mm. On the trigger day, serum progesterone levels were assessed in the patients. Thirty-six hours post-trigger, ovarian follicular fluid was aspirated using a transvaginal ultrasound-guided needle for the purpose of oocyte retrieval. Luteal phase support was initiated on the day of oocyte retrieval with vaginal micronized progesterone (Crinone 8%; Merck Serono) in the patients receiving single euploid ET with fresh blastocysts.
3. Embryo culture protocol and DNA analysis
Sperm were prepared for intracellular sperm injection or insemination using the technique previously described [10]. A four-well dish, containing approximately 400 µL of single-step medium (LifeGlobal), was employed for the cultivation of normally fertilized zygotes displaying two normal pronuclei for several days. Embryonic development was monitored using an EmbryoScope device (Vitrolife AB). The stages of blastocyst development were assessed based on the Gardner classification [11].
TE biopsy and PGS were performed on 522 embryos in the fresh cycle group and 660 embryos in the frozen cycle group. On the 3rd day, all viable embryos underwent zona pellucida perforation in preparation for blastocyst biopsy. This was achieved by creating a small opening in the zona pellucida using a CRONUS 3 laser (400 mW, 0.357 ms pulse width; Light Conversion). After this procedure, the embryos were monitored until days 5 and 6. Only the best-quality blastocyst embryos (of a grade better than 2B) were selected for the procedure, with a preference for the TE embryo biopsy technique. The biopsy timing was determined based on the quality of the embryo, rather than the day of the blastocyst biopsy. The expanded blastocyst, which had by then differentiated into TE cells and an inner cell mass, was biopsied. TE cells herniating from the zona perforation were gently aspirated using a biopsy pipette and separated from the rest of the blastocyst. The tight junctions between the TE cells were severed using two direct laser pulses of 400 mW and 0.4 ms. To facilitate separation, mechanical rubbing on the holding pipette was performed. The biopsied cells were then immediately rinsed in a washing buffer. After rinsing, a polymerase chain reaction tube was prepared with 2 μL of washing buffer, and the cells were loaded into the tube. Each tube containing the TE biopsy was labeled with a number corresponding to the embryo and was sent to the reference genetic lab on dry ice for analysis. Following the biopsy, the blastocysts were immediately vitrified using a vitrification kit and Cryotops (Kitazato). The biopsy specimens obtained from the blastocysts were analyzed using 24-chromosome array comparative genomic hybridization (aCGH) (Reprogenetics LLC), following the method previously outlined [12].
Single euploid ET, either fresh or frozen-thawed, was scheduled to be performed once the aCGH results were obtained. For the fresh strategy, the biopsy of expanded blastocysts was conducted at 10:00 AM on the 5th day. While the results were pending, the embryos were cultured overnight until midday on the 6th day, in preparation for fresh ET of the euploid embryos.
The schedule for frozen-thawed ET was set to follow the patient’s subsequent menstrual cycle, with endometrial preparation involving a daily oral dose of 6 mg estradiol valerate from the 2nd to the 11th day of the cycle. On the 11th day, the thickness of the endometrial tissue was measured using transvaginal ultrasound. In cases in which the endometrium was more than 7 mm thick, the 6 mg estradiol valerate treatment was maintained. On the 14th day of the cycle, vaginal progesterone (Crinone 8% gel) was incorporated into the treatment regimen. The frozen-thawed ET was performed on either the 5th or 6th day of the progesterone adjustment. Both the estrogen and progesterone treatments were sustained until week 10 of pregnancy.
Ten days following ET, the concentration of hCG was assessed, with a value exceeding 10 IU/L considered positive. The implantation rate was calculated by dividing the number of gestational sacs observed via ultrasonography by the number of transferred embryos. A clinical pregnancy was defined as the presence of an intrauterine sac and detectable fetal heart activity. Any pregnancy that continued beyond week 10 of gestation was classified as an ongoing pregnancy.
4. Statistical analysis
The collected data were statistically evaluated using SPSS version 15.0 (SPSS Inc.). For the analysis of non-normally distributed metric variables, the Kruskal-Wallis test and the Mann-Whitney U test were employed. The t-test was utilized for the analysis of normally distributed variables. Categorical variables were presented as numbers and percentages, and the chi-square test or its derivatives were used to compare these variables between the groups. A p-value of <0.05 was considered to indicate statistical significance. Unless otherwise specified, the values were expressed as mean±standard deviation.
Results
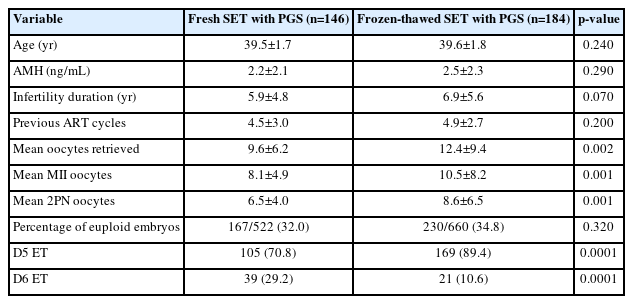
We examined a total of 330 patients, aged between 38 and 43 years, who underwent either single fresh or frozen-thawed ET on day 5 or 6 with TE biopsy. Table 1 provides the baseline characteristics of the study groups.
No statistically significant difference was observed in terms of age, anti-Müllerian hormone levels, duration of infertility, and previous ART cycles between the fresh and frozen-thawed ET groups. The numbers of retrieved oocytes, metaphase II oocytes, and fertilized (two-pronuclear) oocytes were greater in the frozen-thawed embryo group. The percentage of euploid embryos was comparable between the groups, with 167 of 522 embryos (32%) in the fresh ET group and 230 of 660 embryos (34.8%) in the frozen ET group being euploid (p=0.32).
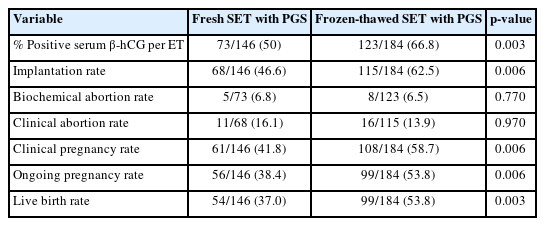
Table 2 presents the clinical outcomes of the patients. The rate of positive serum β-hCG per ET was lower for fresh single embryo transfer (SET) with PGS than for frozen-thawed SET with PGS (50% vs. 66.8%, p=0.003). Additionally, the implantation rates were lower for fresh transfer than for frozen-thawed transfer (46.6% vs. 62.5%, p=0.006). However, no significant differences were observed between the groups in terms of abortion rates, either biochemical (fresh 6.8 vs. frozen, 6.5%, p=0.77) or clinical (fresh, 16.1% vs. frozen, 13.9%, p=0.97). The rates of clinical pregnancy (41.7% vs. 58.7%, p=0.006), ongoing pregnancy (38.4% vs. 53.8%, p=0.006), and live birth (37.0% vs. 53.8%, p=0.003) were higher in the frozen-thawed group.
Discussion
PGS is the key strategy promoting the clinical success of ART cycles in AMA patients. An additional method to improve pregnancy rates involves the use of ET with a euploid embryo. In the present study, the rates of clinical pregnancy, ongoing pregnancy, and live birth were statistically higher in the group of AMA patients who underwent frozen rather than fresh ET.
At present, the strategy of frozen-thawed ET is gaining popularity due to its association with improved implantation and pregnancy rates. The success of frozen ET is critically dependent on optimal endometrial preparation, as evidenced by the suboptimal results observed with the fresh ET strategy. This underscores the importance of endometrial receptivity and the implantation window [13]. A review study by Evans et al. [8] indicated that endometrial receptivity was diminished during COH cycles, while frozen ET yielded more favorable outcomes for both mother and baby. Roque et al. [14] conducted an analysis of 530 cycles, comparing the outcomes of fresh and frozen transfers. They reported a relative risk (RR) of 1.33 for the implantation rate and 1.28 for the ongoing pregnancy rate in the frozen group. The study also suggested that implantation failure could be attributed to COH [14]. A systematic review of three randomized controlled trials involving a total of 633 women found that both the clinical pregnancy rate (RR, 1.31; 95% confidence interval [CI], 1.10 to 1.56) and ongoing pregnancy rate (RR, 1.32; 95% CI, 1.10 to 1.59) were higher in the elective frozen ET group compared to the fresh ET group. However, the review found no significant difference in miscarriage rates (RR, 0.83; 95% CI, 0.43 to 1.60) [15]. The practice of freezing all embryos ensures that all blastocysts are considered for transfer, which leads to a higher proportion of successful ETs [9]. A recent study by Coates et al. [9] revealed that frozen-thawed euploid ET following PGS resulted in superior pregnancy outcomes. Our study similarly indicated that AMA patients experienced higher implantation and pregnancy rates with frozen single euploid ET.
It is well-established that the success rate of ART tends to decrease substantially in women aged 40 years and older. The decline in fertility within this age group is primarily attributed to the heightened risk of age-related aneuploidy [1]. In a retrospective study conducted by Lee et al. [10], AMA and ART outcomes were analyzed. The average participant ages were 41.2 and 41.3 years for the two study groups. Biopsies were performed on 451 blastocysts in the PGS group (n=170). Ploidy analysis revealed that 20.4% of the blastocysts were euploid, while 74.3% exhibited aneuploidy. Of the remaining blastocysts, 3% could not be diagnosed, and 2.2% displayed chaotic profiles post-amplification. Both implantation rate and live delivery rate per transferred embryo were significantly higher in the PGS group [10]. In a pilot study, Ma et al. [16] examined rapid aCGH in the selection of blastocysts for fresh SET and compared the results with methods involving a vitrified ET cycle. Despite the small sample size (eight for the fresh and 13 for the frozen group) and the non-randomized nature of the study, success was observed in the clinical pregnancy rate, at 87.5% in the fresh transfer group and 76.9% in the frozen ET group [16]. Capalbo et al. [6] demonstrated that aneuploidy rates were significantly higher in women of advancing age (odds ratio, 1.12). Pregnancy rates were 57.3% and 75.6% in euploid ET for average ages of 38.8 and 36.1 years, respectively [6]. For euploid embryos, the implantation potential was higher in AMA patients [10]. In fresh and frozen-thawed cycles, a single selective euploid ET was associated with an increased pregnancy rate [6,15]. Furthermore, a single euploid ET reduced the likelihood of multiple pregnancies, which are associated with higher abortion rates and premature deliveries with newborn complications. In the present study, we opted for a SET strategy in both groups, and the euploid embryo rates were similar between the groups. The primary difference between groups was the transfer strategy, with endometrial receptivity being crucial for implantation. Our findings revealed high implantation rates in the frozen ET group.
In the literature, many studies have been conducted to compare the outcomes of fresh and frozen ET [15]. However, the numbers and sample sizes of studies comparing these two transfer strategies with euploid embryos are limited. Although the present study was retrospective, it had the largest participant pool to date for a comparison of fresh versus frozen ET for euploid embryos. Only one prospective randomized controlled study has been conducted to investigate these two ET strategies for euploid embryos. This was carried out by Coates et al. [9], analyzing fresh versus frozen transfers after PGS with next-generation sequencing in a total of 184 patients. The average number of embryos transferred was 1.4 for the fresh ET group and 1.5 for the frozen ET group (p=0.27). Ongoing pregnancy rates (62.2% vs. 40.9%) and live birth rates (61.5% vs. 39.8) were significantly higher in the freeze-all group compared to the fresh group (p<0.01 and p<0.01, respectively). The results were significantly more favorable in the frozen ET group than in the fresh group according to the subgroup analysis of day-5 biopsied euploid blastocysts; however, the difference was not significant. The authors attributed this result to the small sample size. Our study included 330 participants and revealed that ongoing pregnancy rates and live birth rates were significantly higher in the frozen group. Although this study is the first to select the SET strategy between fresh or frozen, the results were comparable with the findings of Coates et al. [9]. The most influential factors impacting the success of ART are the embryo and the endometrium. A higher estrogenic environment has also been found to potentially lead to reduced endometrial receptivity and poorer pregnancy outcomes [15]. Our study considered all of these factors to examine the effect of the endometrial factor alone on pregnancy outcomes. In our findings, the strategy of frozen-thawed single euploid ET resulted in higher implantation and pregnancy rates compared to fresh single euploid ET. Additionally, this transfer strategy lowers the risk of ovarian hyperstimulation syndrome and multiple pregnancies, which are serious conditions with high morbidity and mortality rates in ART.
In conclusion, the present study suggests that the use of frozen-thawed single euploid ET allows sufficient time for comprehensive genetic evaluation, while also enhancing implantation and pregnancy rates relative to fresh single euploid ET in AMA patients undergoing PGS. This research is the most comprehensive to date in comparing these two treatment protocols, and it is the first to employ a single euploid transfer to mitigate the impact of the embryo factor on the success of ART. Our results indicate a trend favoring the strategy of frozen-thawed single euploid ET. However, to better understand ART outcomes, additional prospective randomized controlled studies involving larger groups may be necessary.
Notes
Conflict of interest
No potential conflict of interest relevant to this article was reported.
Author contributions
Conceptualization: FO, GO, SK. Data curation: FO, GO. Formal analysis: FO. Methodology: FO, GO, SK. Writing-original draft: FO. Writing-review & editing: YS, HY.