|
 |
- Search
| Clin Exp Reprod Med > Volume 44(2); 2017 > Article |
Abstract
Objective
Sperm morphology plays an important role in infertility, especially in cases of defects in the heads of spermatozoa. Tapered-head or elongated-head spermatozoa are examples of morphological abnormalities. The aim of this study was to compare the semen parameters, levels of protamine deficiency, and frequency of apoptosis between patients with normozoospermia and those with teratozoospermia with tapered-head spermatozoa.
Methods
Fifty-two semen samples (27 patients with tapered-head sperm and 25 fertile men) were collected and semen analysis was performed according to the World Health Organization criteria for each sample. Protamine deficiency and the percentage of apoptotic spermatozoa were evaluated using chromomycin A3 (CMA3) staining and terminal deoxynucleotidyl transferase dUTP nick-end labelling (TUNEL) assays, respectively.
Results
Sperm concentration, motility, and normal morphology in the tapered-head spermatozoa (cases) were significantly lower than in the normozoospermic samples (controls). CMA3-reactive spermatozoa (CMA3+) in the case group were more common than in the controls. Apoptotic spermatozoa (TUNEL-positive) were significantly more common in the cases than in the controls.
Half of infertility cases are related to male factors, and 30% are limited to male factor infertility [1]. The first step of male infertility assessment is seminal fluid analysis, which consists of a sperm count and an analysis of motility and morphology, which provide valuable information on a patient's fertility status. Abnormalities in each of mentioned parameters are referred to oligozoospermia, asthenozoospermia, and teratozoospermia, respectively, as well as azoospermia [2,3]. Sperm morphology is an important semen parameter, and is considered to be a reliable index of the quality of spermatogenesis and subsequent fertility [4]. Human sperm morphological defects include a wide variety of unusual sperm shapes in the head, neck, midpiece, and tail. Previous studies have documented a relationship between abnormal sperm morphology and fertility potential [5]. The cut-off value for the normality of sperm morphology is 4% according to the last version of the World Health Organization (WHO) criteria [6]. Teratozoospermia is expressed as the percentage of atypical sperm phenotypes present in a sample, which is a good predictor for male fertility with or without the use of assisted reproductive technology [7,8,9]. Tapered-head spermatozoa are considered to have a sperm morphological defect caused by a temporary defect in Sertoli cell ectoplasmic specialization and the acroplaxome involved in nuclear formation [10].
However, spermatogenesis is a unique and complicated process, in which 80% to 85% of histones are replaced by protamine in human spermatozoa, and only 15% to 20% of testicular histones remain intact. Intermolecular and intramolecular disulphide bond formation in sperm protamines cause chromatin condensation and morphological changes in spermatids, leading to the formation of mature and differentiated spermatozoa with condensed nuclei that exhibit normal head morphology [11]. It is clear that S-S bonds are essential for sperm chromatin stability, and any reduction in S-S bonds due to protamine deficiency makes the chromatin more susceptible to denaturation [12]. Previous studies have reported a significant relationship between morphological defects in spermatozoa and their DNA integrity [13,14,15].
To the best of our knowledge, there are insufficient data on the evaluation of sperm chromatin abnormalities in patients with tapered-head spermatozoa. Thus, the aim of the present study was to investigate the possible relationship between sperm protamine deficiency and the rate of apoptosis in the percentage of tapered-head sperm cells in infertile men.
In this case-control study, semen samples were collected from 52 men referred to our andrology lab at the Research and Clinical Center for Infertility in Yazd, Iran. The patients were recruited between August 2015 and February 2016. The patients were divided into two groups: 27 teratozoospermic infertile patients comprised the case group and 25 normozoospermic fertile men comprised the control group. A comprehensive evaluation to establish the aetiology of infertility was conducted, including a physical examination, smoking history, cytogenetic tests, and immunological and reproductive hormonal assays. The inclusion criteria for patients were the presence of 40% to 100% of sperm cells with tapered-head morphology (at least two times less wide than the normal shape) in their semen. An infertile man was defined as a man who had no child after a period of unprotected intercourse of more than 1 year. A control group included fertile donors who had fathered at least one child during the past 12 months and had normal semen parameters according to the 2010 WHO criteria [16]. Heavy smokers (more than a pack of cigarettes per day during the past year), drug addicts, alcohol consumers, men with history of varicocele, and men aged more than 45 years were excluded from the study. This study was approved by the ethics committee of the Yazd Research and Clinical Center for Infertility, and informed consent forms were signed by all participants.
Semen samples were collected by masturbation after 2 to 5 days of sexual abstinence. Each specimen was allowed to undergo liquefaction, and then was evaluated for sperm concentration, motility, and morphology according to the 2010 WHO criteria [16]. Briefly, sperm motility was assessed manually by phase-contrast microscopy (Axiostar Plus; Zeiss, Göttingen, Germany) at ×400 magnification, with sperm classified as showing progressive motility (grade A), non-progressive motility (grade C), or being immotile (grade D). Papanicolaou staining was applied to evaluate morphological abnormalities, and at least 200 sperm cells were examined per slide. Sperm count was assessed using a Makler counting chamber (Sefi Medical, Haifa, Israel) [17]. All analyses were performed by a single experienced laboratory technician blinded to the study protocol.
Chromomycin A3 (CMA3) (Sigma, St. Louis, MO, USA) is a fluorochrome specific for guanosine and cytosine-rich sequences, and is used to evaluate the degree of protamination of chromatin in sperm [17]. At least 200 spermatozoa were counted under fluorescence microscopy (BX51; Olympus, Tokyo, Japan) with a 460-nm filter and ×100 eyepiece magnification. The percentages of spermatozoa with bright yellow heads (CMA3+) and without brightness (CMA3−) were determined and reported as percentages [18].
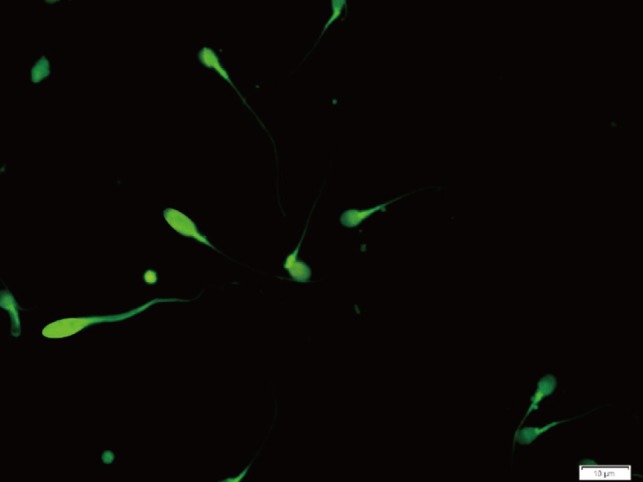
The percentage of apoptotic spermatozoa in each sample was determined by terminal deoxynucleotidyl transferase dUTP nick-end labelling (TUNEL) assays using an In Situ Cell Death Detection kit (Roche Diagnostics, Mannheim, Germany) under fluorescent microscopy; normal DNA was detected as light green and damaged DNA was seen as bright green [19].
SPSS ver. 20.0 (IBM Corp., Armonk, NY, USA) was used for all data analysis. Data were expressed as mean±standard deviation. Differences between variables with a normal distribution were analysed using the Student t-test and abnormally distributed data were assessed using the nonparametric Mann-Whitney U test. A p-value <0.05 was considered to indicate statistical significance.
In this research, a total of 52 semen samples were studied in two groups. The mean age was 35.41±6.5 years in cases and 34.36±5.4 years in the control group.
Sperm parameters, including sperm count, motility (rapid [grade A], slow [grade B], non-progressive [grade C], or immotile sperm [grade D]), and sperm morphology, in the two groups are presented in Table 1. Sperm count, motility (grades A, B, C), total motility, and sperm morphology were significantly lower in the cases than in the controls (p<0.003). Immotile sperm (grade D) were significantly less common in the control group (p<0.001).
In the sperm apoptosis assessment, after TUNEL assays and the application of fluorescent microscopy, the percentage of apoptotic sperm (TUNEL+) was found to be 42.57%±18.02% and 9.03%±2.94% in the case and control groups, respectively, which was a significant difference (p=0.004) (Table 2, Figure 2).
The Pearson correlation test indicated that there was no significant relationship between semen parameters and sperm chromatin integrity or sperm apoptosis in the cases.
Abnormal sperm morphology is correlated with nuclear chromatin integrity and consequent infertility [13]. In this study, we assessed protamine deficiency and sperm apoptosis in infertile men with tapered-head spermatozoa using CMA3 and TUNEL assays. We hypothesized that tapered-head sperm would have higher rates of protamine deficiency and apoptosis. The results showed significant differences between the two groups regarding sperm protamine deficiency. In agreement with our findings, it has been reported that DNA fragmentation was significantly more common in tapered-head sperm than in fertile controls. The TUNEL assay, which was applied in this study, has been used to show that the incidence of round-headed sperm was positively correlated to the level of DNA fragmentation. In addition, sperm with tapered heads have been directly correlated to round-headed sperm [10]. Similarly, a previous study demonstrated that the morphology of sperm selected for intracytoplasmic morphologically selected sperm injection was associated with DNA integrity, as determined using a sperm chromatin dispersion test [15]. Mangiarini et al. [14] described multiple sperm morphological defects and their correlation with the DNA fragmentation index using high-power magnification. As they documented, sperm with a vacuolated head, non-oval head, or a tapered head had a different DNA fragmentation index than morphologically normal sperm. Furthermore, tapered sperm were less likely to show positive results on a TUNEL test than vacuolated-head or small non-oval-head spermatozoa. Moreover, DNA fragmentation has been reported to be an important factor affecting sperm quality. Sperm DNA defects have been proven to have a negative effect on fertilization, implantation, embryo development, and even the health of offspring both in vivo and in vitro [20,21]. In fact, the injection of sperm with abnormal morphology, including an atypical head, elongated head, or amorphous cytoplasmic droplets has been found to lead to the formation of low-fertility-potential embryos, as well as low implantation and pregnancy rates [15,22].
Regarding apoptosis, we found a significantly higher rate of TUNEL-positive spermatozoa in tapered-head sperm than in normal samples. There is a negative relationship between TUNEL-positive cells and semen parameters, sperm fertilization potential, and embryo cleavage [23]. In our study, the TUNEL assay revealed a significant difference in the apoptosis rate between tapered-head and normal sperm. It has previously been reported that the most TUNEL-positive sperm with DNA fragmentation have defects in the head morphology [24]. Previous studies have also reported that the expression of apoptosis-regulated proteins was increased in pyriform sperm [25]. This may be due to abnormalities in spermiogenesis. Spermiogenic flaws may lead to germ cell apoptosis, resulting in defects in sperm count motility and morphology known as oligo-astheno-teratozoospermia (OAT syndrome) [26]. Furthermore, some antibodies can induce apoptosis and consequent chromatin defects in somatic cells, and these antibodies have been found more than twice as often in OAT patients in comparison with normozoospermic men [27]. Moreover, high concentrations of reactive oxygen species in morphologically abnormal semen samples resulted in elevated nuclear DNA damage [28] and increased apoptosis [29]. Sakkas et al. [30] showed that increased levels of TUNEL-positive spermatozoa and Fas and p53 expression were more common among men with low sperm concentration and poor morphology. In contrast, sperm nuclear DNA protection is not favourable in abnormal semen samples due to the nuclear remodelling process. One of the factors responsible for sperm DNA damage is seminal reactive oxygen species elevation [31,32] in patients with leucocytosis, varicocele, and endogenous inflammation. This is also associated with abnormal sperm morphology [33], and antioxidant therapy could be beneficial for reducing reactive oxygen species-induced injuries and may provide an increased likelihood of fertility [34].
In conclusion, our study using CMA3 and TUNEL tests demonstrated a significant increase in sperm DNA protamine deficiency as well as in the apoptosis rate in patients with tapered-head sperm, and these forms of damage may affect the quality of the ejaculated spermatozoa and decrease their fertility potential both in natural cycles and in assisted reproductive technology cycles.
Acknowledgments
The authors especially thank Jalal Ghasemzadeh for his technical assistance during this research. This work was adapted from the master's student thesis.
Notes
References
1. Kierszenbaum AL. Histology and cell biology: an introduction to pathology. 1st ed. St. Louis: Mosby; 2002.
2. Carrell DT, Emery BR, Hammoud S. Altered protamine expression and diminished spermatogenesis: what is the link? Hum Reprod Update 2007;13:313-327.PMID: 17208950.



3. Correa-Perez JR, Fernandez-Pelegrina R, Aslanis P, Zavos PM. Clinical management of men producing ejaculates characterized by high levels of dead sperm and altered seminal plasma factors consistent with epididymal necrospermia. Fertil Steril 2004;81:1148-1150.PMID: 15066482.


5. Greco E, Iacobelli M, Rienzi L, Ubaldi F, Ferrero S, Tesarik J. Reduction of the incidence of sperm DNA fragmentation by oral antioxidant treatment. J Androl 2005;26:349-353.PMID: 15867002.


6. Tanaka H, Miyagawa Y, Tsujimura A, Matsumiya K, Okuyama A, Nishimune Y. Single nucleotide polymorphisms in the protamine-1 and -2 genes of fertile and infertile human male populations. Mol Hum Reprod 2003;9:69-73.PMID: 12569175.



7. Menkveld R, Stander FS, Kotze TJ, Kruger TF, van Zyl JA. The evaluation of morphological characteristics of human spermatozoa according to stricter criteria. Hum Reprod 1990;5:586-592.PMID: 2394790.



8. Lee RK, Hou JW, Ho HY, Hwu YM, Lin MH, Tsai YC, et al. Sperm morphology analysis using strict criteria as a prognostic factor in intrauterine insemination. Int J Androl 2002;25:277-280.PMID: 12270024.


9. Shibahara H, Obara H, Ayustawati , Hirano Y, Suzuki T, Ohno A, et al. Prediction of pregnancy by intrauterine insemination using CASA estimates and strict criteria in patients with male factor infertility. Int J Androl 2004;27:63-68.PMID: 15149462.


10. Tang SS, Gao H, Zhao Y, Ma S. Aneuploidy and DNA fragmentation in morphologically abnormal sperm. Int J Androl 2010;33:e163-e179.PMID: 19732195.


11. Cheng CY. Molecular mechanisms in spermatogenesis. New York: Springer; 2008.
12. Elinati E, Kuentz P, Redin C, Jaber S, Vanden Meerschaut F, Makarian J, et al. Globozoospermia is mainly due to DPY19L2 deletion via non-allelic homologous recombination involving two recombination hotspots. Hum Mol Genet 2012;21:3695-3702.PMID: 22653751.


13. Kramer JA, Krawetz SA. Genesis of a novel human sequence from the protamine PRM1 gene. Comp Biochem Physiol C Pharmacol Toxicol Endocrinol 1998;120:467-473.PMID: 9827065.


14. Mangiarini A, Paffoni A, Restelli L, Ferrari S, Guarneri C, Ragni G, et al. Specific sperm defects are differentially correlated with DNA fragmentation in both normozoospermic and teratozoospermic subjects. Andrology 2013;1:838-844.PMID: 24115574.


15. Maettner R, Sterzik K, Isachenko V, Strehler E, Rahimi G, Alabart JL, et al. Quality of human spermatozoa: relationship between high-magnification sperm morphology and DNA integrity. Andrologia 2014;46:547-555.PMID: 23692628.


16. World Health Organization. WHO laboratory manual for the examination and processing of human semen. 5th ed. Geneva: WHO Press; 2010.
17. Talebi AR, Moein MR, Tabibnejad N, Ghasemzadeh J. Effect of varicocele on chromatin condensation and DNA integrity of ejaculated spermatozoa using cytochemical tests. Andrologia 2008;40:245-251.PMID: 18727735.


18. Agarwal A, Bragais FM, Sabanegh E. Assessing sperm function. Urol Clin North Am 2008;35:157-171.PMID: 18423237.


19. Talebi AR, Khalili MA, Vahidi S, Ghasemzadeh J, Tabibnejad N. Sperm chromatin condensation, DNA integrity, and apoptosis in men with spinal cord injury. J Spinal Cord Med 2013;36:140-146.PMID: 23809529.



20. Aitken RJ, De Iuliis GN. Value of DNA integrity assays for fertility evaluation. Soc Reprod Fertil Suppl 2007;65:81-92.PMID: 17644956.

21. Bungum M, Bungum L, Lynch KF, Wedlund L, Humaidan P, Giwercman A. Spermatozoa DNA damage measured by sperm chromatin structure assay (SCSA) and birth characteristics in children conceived by IVF and ICSI. Int J Androl 2012;35:485-490.PMID: 21950616.


22. De Vos A, Van De Velde H, Joris H, Verheyen G, Devroey P, Van Steirteghem A. Influence of individual sperm morphology on fertilization, embryo morphology, and pregnancy outcome of intracytoplasmic sperm injection. Fertil Steril 2003;79:42-48.PMID: 12524062.


23. Pradeepa MM, Nikhil G, Hari Kishore A, Bharath GN, Kundu TK, Rao MR. Acetylation of transition protein 2 (TP2) by KAT3B (p300) alters its DNA condensation property and interaction with putative histone chaperone NPM3. J Biol Chem 2009;284:29956-29967.PMID: 19710011.



24. Gandini L, Lombardo F, Paoli D, Caponecchia L, Familiari G, Verlengia C, et al. Study of apoptotic DNA fragmentation in human spermatozoa. Hum Reprod 2000;15:830-839.PMID: 10739828.



25. Shojaei Saadi HA, van Riemsdijk E, Dance AL, Rajamanickam GD, Kastelic JP, Thundathil JC. Proteins associated with critical sperm functions and sperm head shape are differentially expressed in morphologically abnormal bovine sperm induced by scrotal insulation. J Proteomics 2013;82:64-80.PMID: 23500133.


26. Udagawa O, Ito C, Ogonuki N, Sato H, Lee S, Tripvanuntakul P, et al. Oligo-astheno-teratozoospermia in mice lacking ORP4, a sterol-binding protein in the OSBP-related protein family. Genes Cells 2014;19:13-27.PMID: 24245814.


27. Ramos L, van der Heijden GW, Derijck A, Berden JH, Kremer JA, van der Vlag J, et al. Incomplete nuclear transformation of human spermatozoa in oligo-astheno-teratospermia: characterization by indirect immunofluorescence of chromatin and thiol status. Hum Reprod 2008;23:259-270.PMID: 18056059.



28. Koksal IT, Tefekli A, Usta M, Erol H, Abbasoglu S, Kadioglu A. The role of reactive oxygen species in testicular dysfunction associated with varicocele. BJU Int 2000;86:549-552.PMID: 10971290.


29. Cam K, Simsek F, Yuksel M, Turkeri L, Haklar G, Yalcin S, et al. The role of reactive oxygen species and apoptosis in the pathogenesis of varicocele in a rat model and efficiency of vitamin E treatment. Int J Androl 2004;27:228-233.PMID: 15271202.


30. Sakkas D, Moffatt O, Manicardi GC, Mariethoz E, Tarozzi N, Bizzaro D. Nature of DNA damage in ejaculated human spermatozoa and the possible involvement of apoptosis. Biol Reprod 2002;66:1061-1067.PMID: 11906926.



31. Ni K, Steger K, Yang H, Wang H, Hu K, Zhang T, et al. A comprehensive investigation of sperm DNA damage and oxidative stress injury in infertile patients with subclinical, normozoospermic, and astheno/oligozoospermic clinical varicocoele. Andrology 2016;4:816-824.PMID: 27218783.


32. Lobascio AM, De Felici M, Anibaldi M, Greco P, Minasi MG, Greco E. Involvement of seminal leukocytes, reactive oxygen species, and sperm mitochondrial membrane potential in the DNA damage of the human spermatozoa. Andrology 2015;3:265-270.PMID: 25598385.


33. Shi TY, Chen G, Huang X, Yuan Y, Wu X, Wu B. Effects of reactive oxygen species from activated leucocytes on human sperm motility, viability and morphology. Andrologia 2012;44(Suppl 1): 696-703.PMID: 22097888.


34. Palmieri M, Papale P, Della Ragione A, Quaranta G, Russo G, Russo S. In vitro antioxidant treatment of semen samples in assisted reproductive technology: effects of myo-inositol on nemaspermic parameters. Int J Endocrinol 2016;2016:2839041PMID: 27672392.




Figure 1
Chromomycin A3 (CMA3) staining for the evaluation of sperm protamine deficiency. Bright yellow tapered-head sperm cells (CMA3+) show protamine deficiency, and yellowish-green tapered-head sperm cells (CMA3−) show normal protamine content (fluorescence microscopy, ×100 eyepiece magnification).
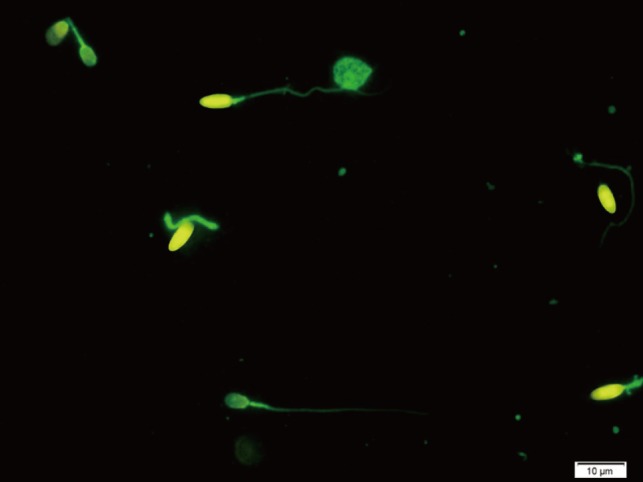
Figure 2
TUNEL assay for the detection of sperm apoptosis. Under fluorescent microscopy, normal DNA (non-apoptotic sperm) is seen as light green, and damaged DNA (apoptotic sperm) is seen as bright green (×100 eyepiece magnification). TUNEL, terminal deoxynucleotidyl transferase dUTP nick-end labelling.